The Greatest Public Health Threat is Here Now — Antibiotic Resistant Diseases
By Bob Aronson
Antibiotics and drugs called antimicrobial agents have been used for the last 70 years to treat patients with infectious diseases who might genotherwise have died. Unfortunately these “Miracle” drugs were used for such a long time and so indiscriminately that the organisms they were designed to kill have mutated and become more resistant to them. In some cases the drugs don’t work at all anymore.
Each year in the United States, at least 2 million people become infected with antibiotic resistant bacteria and at least 23,000 of them die as a result. While 23,000 is a significant number it does not even come close to being in the catastrophic category so there’s not much media attention given to the problem – until now and this headline.
Is Antibiotic resistance: the greatest public health threat of our time?
T his is not the stuff of science fiction. It is real and it is supported by both the World Health Organization (WHO) and by the U.S. Centers For Disease Control in Atlanta, Georgia (CDC)
his is not the stuff of science fiction. It is real and it is supported by both the World Health Organization (WHO) and by the U.S. Centers For Disease Control in Atlanta, Georgia (CDC)
The WHO says we are in a “post-antibiotic era”, in which even the most minor bacterial infections could mean death, a statement made true because of antibiotic misuse, overprescribing and poor diagnoses.
A world without antimicrobials would be a world without modern medicine, so why is there not more urgency in addressing the global rise of drug resistance? The New Statesman brought leading health experts together to discuss the problem. http://www.newstatesman.com/sci-tech/2014/07/antibiotic-resistance-greatest-public-health-threat-our-time
Antibiotic-resistant infections can happen anywhere. The CDC says that most of them happen in the general community; however, most deaths related to antibiotic resistance happen in healthcare settings such as hospitals and nursing homes. http://www.cdc.gov/drugresistance/threat-report-2013/index.html
The Threat to You
Diseases that either are or are becoming antibiotic resistant http://www.cdc.gov/drugresistance/DiseasesConnectedAR.html
A growing number of disease-causing organisms or pathogens, are resistant to one or more antimicrobial drugs—including the bacteria that cause tuberculosis, the viruses that cause influenza, the parasites that cause malaria, and the fungi that cause yeast infections. All are becoming resistant to the antimicrobial agents used for treatment. Curious about other diseases that may not respond to your antibiotics? Here’s a partial list from the CDC. The full list can be seen by clicking on the above link.
Acinetobacter  is a type of gram-negative bacteria that is a cause of pneumonia or bloodstream infections among critically ill patients. Many of these bacteria have become very resistant to antibiotics.
is a type of gram-negative bacteria that is a cause of pneumonia or bloodstream infections among critically ill patients. Many of these bacteria have become very resistant to antibiotics.
Anthrax is a serious disease caused by Bacillus anthracis, a bacterium that forms spores. Anthrax most commonly occurs in wild and domestic mammalian species, but it can also occur in humans when they are exposed to infected animals or to tissue from infected animals or when anthrax spores are used as a bioterrorist weapon. Some strains of B. anthracis may be naturally resistant to certain antibiotics and not others. In addition, there may be biologically mutant strains that are engineered to be resistant to various antibiotics.
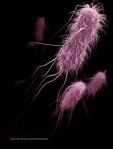 Carbapenem resistant Enterobacteriaceae
Carbapenem resistant Enterobacteriaceae
Untreatable and hard-to-treat infections from carbapenem-resistant Enterobacteriaceae (CRE) bacteria are on the rise among patients in medical facilities. CRE have become resistant to all or nearly all the antibiotics we have today. Almost half of hospital patients who get bloodstream infections from CRE bacteria die from the infection.
Neisseria gonorrhoeae causes gonorrhea, a sexually transmitted disease that can result in  discharge and inflammation at the urethra, cervix, pharynx, or rectum.
discharge and inflammation at the urethra, cervix, pharynx, or rectum.
Group B Streptococcus (GBS) is a type of bacteria that can cause severe illnesses in people of all ages, ranging from bloodstream infections (sepsis) and pneumonia to meningitis and skin infections.
Methicillin-resistant Staphylococcus aureus (MRSA)
Methicillin-resistant Staphylococcus aureus (MRSA) causes a range of illnesses, from skin and wound infections to pneumonia and bloodstream infections that can cause sepsis and death. Staph bacteria, including MRSA, are one of the most common causes of healthcare-associated infections.
Salmonella, non-typhoidal serotypes
Non-typhoidal Salmonella (serotypes other than Typhi, Paratyphi A, Paratyphi B, and Paratyphi C) usually causes diarrhea (sometimes bloody), fever, and abdominal cramps. Some infections spread to the blood and can have life-threatening complications.
 Shigella usually causes diarrhea (sometimes bloody), fever, and abdominal pain. Sometimes it causes serious complications such as reactive arthritis. High-risk groups include young children, people with inadequate hand washing and hygiene habits, and men who have sex with men.
Shigella usually causes diarrhea (sometimes bloody), fever, and abdominal pain. Sometimes it causes serious complications such as reactive arthritis. High-risk groups include young children, people with inadequate hand washing and hygiene habits, and men who have sex with men.
Streptococcus pneumoniae (S. pneumoniae, or pneumococcus) is the leading cause of bacterial pneumonia and meningitis in the United States. It also is a major cause of bloodstream infections and ear and sinus infections.
Tuberculosis (TB) is among the most common infectious diseases and a frequent cause of death  worldwide. TB is caused by the bacteriaMycobacterium tuberculosis (M. tuberculosis) and is spread most commonly through the air. M. tuberculosis can affect any part of the body, but disease is found most often in the lungs. In most cases, TB is treatable and curable with the available first-line TB drugs; however, in some cases, M. tuberculosis can be resistant to one or more of the drugs used to treat it. Drug-resistant TB is more challenging to treat — it can be complex and requires more time and more expensive drugs that often have more side effects. Extensively Drug-Resistant TB (XDR TB) is resistant to most TB drugs; therefore, patients are left with treatment options that are much less effective. The major factors driving TB drug resistance are incomplete or wrong treatment, short drug supply, and lack of new drugs. In the United States most drug-resistant TB is found among persons born outside of the country.
worldwide. TB is caused by the bacteriaMycobacterium tuberculosis (M. tuberculosis) and is spread most commonly through the air. M. tuberculosis can affect any part of the body, but disease is found most often in the lungs. In most cases, TB is treatable and curable with the available first-line TB drugs; however, in some cases, M. tuberculosis can be resistant to one or more of the drugs used to treat it. Drug-resistant TB is more challenging to treat — it can be complex and requires more time and more expensive drugs that often have more side effects. Extensively Drug-Resistant TB (XDR TB) is resistant to most TB drugs; therefore, patients are left with treatment options that are much less effective. The major factors driving TB drug resistance are incomplete or wrong treatment, short drug supply, and lack of new drugs. In the United States most drug-resistant TB is found among persons born outside of the country.
Salmonella serotype Typhi causes typhoid fever, a potentially life-threatening disease. People with typhoid fever usually have a high fever, abdominal pain, and headache. Typhoid fever can lead to bowel perforation, shock, and death.
Vancomycin-Intermediate/Resistant Staphylococcus aureus(VISA/VRSA)
Staphylococcus aureus is a common type of bacteria that is found on the skin. During medical procedures when patients require catheters or ventilators or undergo surgical procedures, Staphylococcus aureus can enter the body and cause infections. When Staphylococcus aureus becomes resistant to vancomycin, there are few treatment options available because vancomycin-resistant S. aureus bacteria identified to date were also resistant to methicillin and other classes of antibiotics.
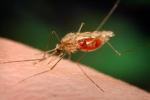 Malaria is a mosquito-borne disease caused by a parasite. People with malaria often experience fever, chills, and flu-like symptoms. The development of resistance to drugs poses one of the greatest threats to malaria control and has been linked to recent increases in malaria morbidity and mortality. Antimicrobial resistance has been confirmed in only two of the four human malaria parasite species, Plasmodium falciparum and P. vivax.
Malaria is a mosquito-borne disease caused by a parasite. People with malaria often experience fever, chills, and flu-like symptoms. The development of resistance to drugs poses one of the greatest threats to malaria control and has been linked to recent increases in malaria morbidity and mortality. Antimicrobial resistance has been confirmed in only two of the four human malaria parasite species, Plasmodium falciparum and P. vivax.
WHO: Antibiotic Resistance Now a ‘Major Threat to Public Health’
Antibiotics are powerful tools for fighting illness and disease, but their overuse has helped create bacteria that are outliving the drugs used to treat them.
Antibiotic resistance is a quickly growing, extremely dangerous problem. World health leaders have described antibiotic-resistant bacteria as “nightmare bacteria” that “pose a catastrophic threat” to people in every country in the world. Many more people die from other conditions that were complicated by an antibiotic-resistant infection.
In addition, almost 250,000 people who are hospitalized or require hospitalization get Clostridium difficile each year, an infection usually related to antibiotic use. C. difficile causes deadly diarrhea and kills at least 14,000 people each year. Many C. difficile infections and drug-resistant infections can be prevented.
How Bacteria Become Resistant
When bacteria are exposed to antibiotics, they start learning how to outsmart the drugs. This process occurs in bacteria found in humans, animals, and the environment. Resistant bacteria can multiply and spread easily and quickly, causing severe infections. They can also share genetic information with other bacteria, making the other bacteria resistant as well. Each time bacteria learn to outsmart an antibiotic, treatment options are more limited, and these infections pose a greater risk to human health.
Infections Can Happen to Anyone, Anywhere
Anyone can become infected with antibiotic-resistant bacteria anywhere and anytime. Most infections occur in the community, like skin infections with MRSA and sexually transmitted diseases. However, most deaths related to antibiotic resistance occur from drug-resistant infections picked up in healthcare settings, such as hospitals and nursing homes.
What you can do to protect yourself against drug-resistant infections
Bob’s Newheart is providing two answers to this question. The first from the CDC and the second from a panel of physician experts who were interviewed for the PBS TV show, Frontline.
CDC Advice
There are many ways you can help prevent the creation and spread of resistance. First, when you are sick, do not demand antibiotics from your doctor or take antibiotics that were not prescribed to you directly for your specific illness. When taking antibiotics, do not skip doses, and make sure to follow the directions about dose and duration from your doctor.
Second, like all diseases, common safety and hygiene methods can prevent disease and spread. Make sure to:
- Get updated and regular vaccinations against drug-resistant bacteria
- Wash your hands before eating and after using the restroom to avoid putting drug-resistant bacteria into your body
- Wash your hands after handling uncooked food to prevent ingesting drug-resistant bacteria that can live on food
- Cook meat and poultry thoroughly to kill bacteria, including potential drug-resistant bacteria
What healthcare providers can do to protect patients from drug-resistant infections (CDC)
 There are many ways to help provide the best care to your patients while protecting them against antibiotic-resistant infections.
There are many ways to help provide the best care to your patients while protecting them against antibiotic-resistant infections.
- Follow all necessary infection control recommendations, including hand hygiene, standard precautions, and contact precautions.
- Diagnose and treat resistant infections quickly and efficiently. Treatment options change often because resistance is complex. Make sure to follow the latest recommendations to ensure you are prescribing appropriately.
- Only prescribe antibiotics when likely to benefit the patient, and be sure to prescribe the right dose and duration.
- Be sure to clearly label dose, duration, and indication for treatment, and include appropriate laboratory diagnostic tests when placing antibiotic orders. This will help other clinicians caring for the patient to change or stop therapy when appropriate.
- Take an antibiotic time out, reassessing therapy after 48-72 hours. Once additional information is available, including microbiology, radiographic, and clinical information, a decision can be made on whether to continue the same therapy.
- When transferring patients, ensure the other facilities are notified of any infection or known colonization.
- Keep tabs on resistance patterns in your facility and in the area around your facility.
- Finally, encourage prevention methods with your patients. Make sure they understand how to protect themselves with vaccines, treatment, and infection control practices such as hand washing and safe food handling.
From PBS “Frontline”
Eight Ways to Protect Yourself from Superbugs
 October 22, 2013, 9:32 pm ET by Sarah Childress
October 22, 2013, 9:32 pm ET by Sarah Childress
Everyone is at risk of becoming infected by drug-resistant bacteria, especially as some have begun to appear outside of hospitals in the general community. So how worried should you be?
The PBS investigative show, “FRONTLINE” asked three infectious disease doctors these questions: what the risks are, how to protect yourself, and what questions to ask when a loved one is in the hospital.
| Dr. Sean Elliott is the medical director of infection prevention at the University of Arizona Health Network | Dr. Brad Spellberg is an infectious diseases specialist at Harbor-UCLA Medical Center | Dr. Wendy Stead is an infectious diseases specialist at Beth Israel Deaconess Medical Center in Boston |
Frontline condensed their advice into eight handy tips to help keep bugs at bay.
Of course, none of this substitutes for actual medical advice. For serious concerns, always consult your doctor.
1. Don’t Panic
Everyone may be at risk, but the chances of catching a drug-resistant bug outside of the hospital are small for most. “For the average healthy person walking down the street? Those organisms are not much of a threat,” Stead says.
“The first principle is to try to live a healthy lifestyle to reduce the need to be in the hospital” where you are more likely to encounter these bugs, Spellberg says. Keep your home and work space clean. Be aware of the food you eat: Wash fruits and vegetables carefully and cook other food properly to reduce your chance of coming into contact with harmful bacteria.
2. Know What to Look For
How do you know if you have a superbug?
“You don’t. And your doctor won’t either, at least at first,” Spellberg said. “The infections caused by antibiotic-resistant bacteria do not cause different symptoms than infections caused by antibiotic-susceptible infections.”
While it’s impossible to give broad advice about so many different kinds of bacteria — and if you’re concerned, you should call your doctor first — there are some signs that an illness might be more serious. “In general, fevers, if they’re accompanied by shaking chills, if they’re getting worse instead of better, that would suggest there’s a bacterial process,” Elliott said.
With community-acquired MRSA, many people first notice a skin infection or boil that becomes larger and more painful, Stead says.
But if you do suspect such an infection, don’t rush to the emergency room, where you might be exposed to other bugs or infect others. Call your primary-care doctor first for advice.
3. Wash Your Hands with Soap and Water. Really wash them. Doctors say they cannot recommend this enough.
“Wash your hands regularly and religiously in the normal times that you would think you should wash them,” Stead says. “Give it a good amount of time” — about 15 seconds — “scrubbing hands thoroughly, not just in and out of the water.”
Turn off the faucet using a paper towel.
Alcohol-based hand-sanitizers are handy too, but remember that one bug, C.Diff, is resistant to that as well. But it does respond to soap and water. So Wash. Your. Hands.
4. Be Careful with the Antibacterial Soap
 The FDA hasn’t determined whether these soaps are more effective than regular soap, and some doctors don’t recommend using them. “You do not need to take ‘antibacterial’ soaps for routine use,” Spellberg says. “There may be specific medical circumstances that warrant special antibacterial cleansers, but these should be prescribed by your physician.”
The FDA hasn’t determined whether these soaps are more effective than regular soap, and some doctors don’t recommend using them. “You do not need to take ‘antibacterial’ soaps for routine use,” Spellberg says. “There may be specific medical circumstances that warrant special antibacterial cleansers, but these should be prescribed by your physician.”
“A lot of the antibacterial soaps are more drying to the skin than would be a simple soap,” Elliott says. “So the more that we break down our skin barriers the higher the risk of getting superimposed bacterial. The real key is the soap and water and the physical action — and keeping hands moisturized. “
5. Ask Your Doctors to Wash Their Hands
“It is every patient’s right to have every health-care provider entering the room to have clean hands,” Elliott says. “We’re supposed to do it, we mandate 100 percent hand- hygiene  compliance, but the reality is that doesn’t happen,” he says.
compliance, but the reality is that doesn’t happen,” he says.
Some hospitals even make health-care providers wear buttons encouraging patients to ask them if they’ve washed their hands. Even if they’re buttonless, you should feel free to ask your providers about it.
“Really — we are not offended by that,” Stead says.
6. Get A Flu Shot
“When people get influenza, they actually become at higher risk as they recover for complicating bacterial infections,” Stead says, because people with weakened immune systems are more vulnerable to other bugs.
“Community-acquired MRSA is a big risk in patients who have recently had influenza,” she notes. “They get influenza and they start to get better, and then the staph comes in. … That’s life threatening. They wouldn’t have been at risk for that if they hadn’t had influenza in the first place.”
7. Ask Whether You Need that Antibiotic
Doctors sometimes feel pressured by patients or their families to prescribe an antibiotic, even if it’s not necessary. Don’t assume you need one — antibiotics don’t work on viral infections like colds or the flu. If your doctor does recommend one, ask whether you really need it.
“Using antibiotics does kill off non-resistant bacteria in your body and makes you likely to acquire antibiotic-resistant bacteria in their place,” Spellberg says. “If your doctor says that they think your infection is probably caused by bacteria and that you do need an antibiotic, ask, ‘Do I need a broadly active antibiotic, or can I take a narrower antibiotic?’ The broader the antibiotic, the more damage to your normal bacteria can be caused. We want physicians to try to prescribe antibiotics that are as narrow as possible for a given infection.”
8. Advocate for Loved Ones in the Hospital
![]() One of the ways drug-resistant bacteria spreads in hospital is through tubes inserted in the body, such as catheters. If someone you care about is on such a device, don’t be afraid to ask doctors whether they still need it, and when the tubes can come out.
One of the ways drug-resistant bacteria spreads in hospital is through tubes inserted in the body, such as catheters. If someone you care about is on such a device, don’t be afraid to ask doctors whether they still need it, and when the tubes can come out.
“Hospitals are much more aggressive about removing things if they’re not needed anymore,” Stead says. “But having patients be aware and try to get things out too is good.”
“Every day that decision needs to be made: Do these things need to stay in or do they need to come out?” Elliott says. The key, he says, is “empowering patients or their advocates to stand up for their health-care needs.”
Conclusion
While physicians and health care workers have a responsibility to provide the best health care, patients also have some responsibility for their own well-being and it boils down to being informed and not being afraid to ask tough questions.
Most of us don’t like challenging physicians, we just assume that will all those many years of education and the raft of framed diplomas on the wall that they must know what they are doing, but the practice of medicine is as much art as it is science. That means even highly educated medical experts can come to the wrong conclusions, so it is extremely important for patients to expand their knowledge of the conditions to which they are exposed or have contracted, ask tough, knowledgeable questions and then, demand clear unequivocal answers. Doing so could mean the difference between life and death.
-0-
 Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s over 4,000 member Organ Transplant Initiative (OTI) and the author of most of these donation/transplantation blogs. You may comment in the space provided or email your thoughts to me at bob@baronson.org.
Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s over 4,000 member Organ Transplant Initiative (OTI) and the author of most of these donation/transplantation blogs. You may comment in the space provided or email your thoughts to me at bob@baronson.org.
Bob’s Newheart was established to support and help everyone, but particularly those who need or have had organ transplants. Some of our blogs are specifically related to donation/transplantation issues while others are more general, but they are all related. Because anti-rejection drugs compromise immune systems, transplant recipients are more susceptible to a variety of diseases. We provide general health and medical information to help them protect themselves while at the same time, helping others live healthier lives and avoid organ failure.
Bob’s Newheart mission is three-fold; 1) to provide news and information that promotes healthier living so people won’t need transplants; 2) To help recipients protect their new organs and; 3) to do what we can to ensure that anyone who needs an organ can get one. About 7,000 Americans die every year while waiting for a life-saving organ. I am sure you will agree that should not happen.
In the U.S. the great majority of people support organ donation, but only about 40% of us officially become organ donors. Many have good intentions but just don’t get around to it. It is hard to accept, but no one knows how long they will live. My transplanted heart came from a 30 year old man. I’m sure he had no intention of being a donor at that age. If you are not yet a donor, please register at www.donatelife.net it only takes a few seconds. Then, tell your family so there is no confusion when the time comes to donate. One organ donor can save or positively affect the lives of up to 60 people. There is no nobler thing you can do than becoming an organ donor.
Bob Aronson
Founder of Bob’s Newheart
Established November 3, 2007
Posted on October 31, 2014, in Health care and tagged anti-rejection, antibiotics, bacteria, compromised immune system, deaths, diseases, infections, organ donation, transplantation, viruses. Bookmark the permalink. 1 Comment.

Pingback: The unconquered enemy | Find Me A Cure