Blog Archives
From the Bottom of My Donor’s Heart. My 20 Year Transplant Journey
Introduction
Overall my transplant has been a very positive experience, but that does not suggest that there weren’t some difficulties and challenges along the way. There were several and they were discouraging, but we kept forging ahead because the alternative was much worse. Now some 20 years post diagnosis. I am alive, I am enjoying life and I am the most grateful recipient on earth. Despite all the setbacks, the bad moments, the complications, I would not hesitate to make the same decision all over again. Thank you Mayo, donor family, my wife and family and the many friends I had and have collected since I got a new heart.
This is an accurate although abbreviated record of my journey. Yours may be totally different and likely will be. I have posted it because of a good many requests to do so. I hope it is helpful to someone. I also hope you will notice that I found some of the experience to be downright funny and I included them because seeing the humor in life’s challenges is important to your recovery. Don’t ever lose your sense of humor; in fact you should aggressively look for it in every situation. It will make your life so much easier to live.
Bob Aronson, heart recipient August 21, 2007 Mayo Clinic, Jacksonville, Florida.
The Beginning. An Earthquake Swallows You Whole
Getting an organ transplant is an experience that few ever have. From the time you first learn that you need one, until a good while after you have one, the ride is not unlike the wildest, highest, steepest, fastest, scariest roller  coaster ride you can imagine. It is like standing in the street when an earthquake hits and the fissure in the pavement runs right between your feet. You get the same feeling you did in that recurring nightmare where no matter how fast you run, your legs feel like rubber and you keep falling, but each time you do it is harder to get up and that something that is chasing you is getting closer. You know you are going to die.
coaster ride you can imagine. It is like standing in the street when an earthquake hits and the fissure in the pavement runs right between your feet. You get the same feeling you did in that recurring nightmare where no matter how fast you run, your legs feel like rubber and you keep falling, but each time you do it is harder to get up and that something that is chasing you is getting closer. You know you are going to die.
Emotions can range from terror, to giddiness, to depression, anxiety, guilt, anger and every other imaginable high, low or even fantasy. An organ transplant will introduce you to feelings you did not know you had and to realities you did not know existed. Most importantly it will allow you to see your own humanity; your strengths, weaknesses vulnerabilities, fears and inadequacies. In other words, you will get to know a side of yourself that you didn’t know existed.
All of us know that someday we will cease to exist, but no one likes talking  about it. Insurance companies like to say, “If something happens to you,” and we all know they don’t mean winning the lottery or getting your very own magic Genii who will pop out of a jar and grant you anything you want. “If something happens to you” means not if, but when you die. It means dead, lifeless, no heartbeat, no breathing, no pulse – DEAD!
about it. Insurance companies like to say, “If something happens to you,” and we all know they don’t mean winning the lottery or getting your very own magic Genii who will pop out of a jar and grant you anything you want. “If something happens to you” means not if, but when you die. It means dead, lifeless, no heartbeat, no breathing, no pulse – DEAD!
When you are told that an organ is failing, you are being told that the last option available to keep you alive is a transplant. You are dying. That is information with which it is hard to come to grips, and those of us who have had transplants have all heard that message loud and clear, it is inevitable. It is a sad fact, but everyone on the transplant list is dying.
I’m sure the death message is never delivered in the same manner twice because the circumstances that lead up to it are all different. The very first recognition that something is wrong is usually met with disbelief. “It’s probably nothing, maybe a false positive, it can’t be organ failure.”
In my case it was in mid-1995 when I left the office late one night after a long day. I’m an asthmatic and I had struggled for air all day. I could hardly wait it for it to end but I had a client until 9 PM. When she left, I waited until the elevator doors closed, turned out the lights, locked the door and took an elevator down six floors to the parking ramp. I had arrived at the office late in the day because of meeting and had to park at the very back of the ramp, a good block from the elevator. Most of the cars were gone now and there wasn’t a living, breathing soul to be seen. I could see my car in the distance, but it may as well have been in the next county. My breathing was so labored I doubted I could make it that far, but I had to try.
I am one of those guys who makes a decision and never looks back, so I forged ahead. I was going to make it to my car no matter what. I thought that if I walked slowly I  wouldn’t use as much air so that’s what I did, but breathing was getting more and more difficult and my rescue inhaler seemed to have no effect. I chalked it up to a defective device and pushed on while carrying a full briefcase. I leaned on cars, support columns and sign posts, but stopped often and fell twice when my legs gave way under me.
wouldn’t use as much air so that’s what I did, but breathing was getting more and more difficult and my rescue inhaler seemed to have no effect. I chalked it up to a defective device and pushed on while carrying a full briefcase. I leaned on cars, support columns and sign posts, but stopped often and fell twice when my legs gave way under me.
By the time I got to my car my suit pants were torn from falling, my hands were scraped and bloodied from using them to break my falls and I was soaking wet from perspiration. With great effort I made it into the car, turned on the AC and just sat there hoping the rest would restore my ability to breathe. It didn’t. I called home to alert my wife that I was in distress and would pick her up on the way to a nearby community hospital ER. She said I should go to a bigger hospital, but I knew the bigger facility would be crowded and the wait would be a long one so we went to the small one. She was right and i was wrong. here’s what happened.
It was a small hospital in Hastings,Minnesota and there were no patients waiting in the ER lobby  when I stumbled to the desk and gasped, “I’m having an asthma attack and need a shot of epinephrine,” and collapsed on a chair next to the nurse.
when I stumbled to the desk and gasped, “I’m having an asthma attack and need a shot of epinephrine,” and collapsed on a chair next to the nurse.
She took my vitals, listened to my chest, looked at my eyes and fingernails, poked around my ankles and said, “This is no asthma attack.” Somehow she alerted a crash team which appeared in microseconds. They brought with them a gurney upon which they c arefully placed me and removed my tie, shirt and t-shirt while wheeling me into an ER exam cubicle. Then, someone else came along and stuck some leads on my chest, sides, legs and arms and wired me to a machine. Another person started an IV. A portable X-ray machine materialized, someone gave me a nitroglycerine pill to place under my tongue but still no shot of epinephrine and I was getting angry. I knew what to do. “Why didn’t they know? I wondered”
arefully placed me and removed my tie, shirt and t-shirt while wheeling me into an ER exam cubicle. Then, someone else came along and stuck some leads on my chest, sides, legs and arms and wired me to a machine. Another person started an IV. A portable X-ray machine materialized, someone gave me a nitroglycerine pill to place under my tongue but still no shot of epinephrine and I was getting angry. I knew what to do. “Why didn’t they know? I wondered”
A doctor appeared, examined me and ignored my repeated requests for epinephrine. Finally he said, “Mr. Aronson this is not an asthma attack, even though you think it is. It’s your heart.” He left the room to have a conversation in the hall with a couple of other people and then returned to say, “Mr. Aronson, we have determined that your condition could best be handled by a  hospital that has cardiologists on duty and specializes in situations just like this. We are sending you there by ambulance so you will get the best and most immediate care possible,” and they wheeled me out to my ride.
hospital that has cardiologists on duty and specializes in situations just like this. We are sending you there by ambulance so you will get the best and most immediate care possible,” and they wheeled me out to my ride.
Too much was happening too fast. I was totally confused. “This is asthma, for heaven’s sake,” I thought. I just couldn’t wrap my mind around this heart stuff. I was 56 years old and thought I was in very good health. I didn’t drink or smoke and was in fairly good physical condition.  I just couldn’t figure out why they thought it was my heart when I knew it was asthma. The ride to United Hospital in St. Paul, Minnesota took about 20 minutes, and I was rushed into their heart unit. More wires, more machines, more activity, blood drawn, questions asked and injections given.
I just couldn’t figure out why they thought it was my heart when I knew it was asthma. The ride to United Hospital in St. Paul, Minnesota took about 20 minutes, and I was rushed into their heart unit. More wires, more machines, more activity, blood drawn, questions asked and injections given.
Another technician appeared with an echocardiogram machine. He placed more leads on my body, some cold gel and began moving a wand around the left side of my chest. In the meantime my breathing was improving.
I could see my heart on the echo monitor and hear the “gulp, swish, swish, g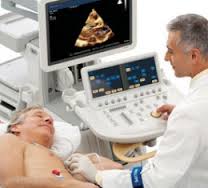 ulp” of the machine. All the while the medical team was explaining every detail of what they were doing and I heard none of it. “It’s an asthma attack,” I kept thinking. And then I lost consciousness.
ulp” of the machine. All the while the medical team was explaining every detail of what they were doing and I heard none of it. “It’s an asthma attack,” I kept thinking. And then I lost consciousness.
I awakened the next morning in a hospital room with my family surrounding me. Everyone was solemn and one of my daughters was crying. A man walked in, he looked like he just stepped off the cover of Gentleman’s Quarterly. “I’m Dr. Thomas Johnson, a cardiologist,” he said. “It appears as though you have a very serious heart condition called Cardiomyopathy. We are going to run some further tests, but you may need a heart transplant.”
I thought, “Boy, this guy doesn’t mince words – a heart transplant? I vaguely remembered being on the air and reporting on the story when Dr. Christian Barnaard performed the first ever in 1967 in a South African hospital. I remember thinking, “Wow, what a development. It will help a whole lot of people someday,” never considering for a moment that I might be one of them. The diagnosis was official now, I had Idiopathic, Dilated Cardiomyopathy. That means I had heart failure from no apparent cause.
It all came together at that moment. The great truth that I had continually denied and avoided was now perfectly clear. The feeling was like that you experience when a monstrous thunder clap or earthquake rattles your bones. It was like lightning bolts flashed out of the clouds, thunder rumbled louder than I could bear and the realization that asthma had nothing to do with my condition that shook my foundation. I was in serious trouble. I felt a mixture of shock, anger, terror, doubt and disbelief. That was my introduction to a process that would take 12 more years before I got a new heart.
The Disease Progresses
A measure of the health of your heart is its ejection fraction (EF). It is how  much blood is pumped out of the heart with each beat. On average we pump out about 60-70 percent. My EF was 25. When it gets too low that means that the heart has to grow larger to hold the retained blood, but it’s a gradual process. For a long while I felt OK. I went about my work and with the help of medication performed as I always had. I was a communication consultant helping business executives with presentations, testimony, personal communication and media interviews, and was always upbeat and energetic. Often I was hired as a keynote speaker at conventions. I never stood behind a lectern, but rather walked around the stage, invading people’s space and getting them involved. Slowly that became harder to do.
much blood is pumped out of the heart with each beat. On average we pump out about 60-70 percent. My EF was 25. When it gets too low that means that the heart has to grow larger to hold the retained blood, but it’s a gradual process. For a long while I felt OK. I went about my work and with the help of medication performed as I always had. I was a communication consultant helping business executives with presentations, testimony, personal communication and media interviews, and was always upbeat and energetic. Often I was hired as a keynote speaker at conventions. I never stood behind a lectern, but rather walked around the stage, invading people’s space and getting them involved. Slowly that became harder to do.
In 1996, a year later, I started to feel a little fatigue and while still energetic I had lost a step or two, but it was barely noticeable. That same year Avis, my wife of 33 years was diagnosed with lung cancer. She fought hard and for a while it looked like she had it beat but in 1998 she succumbed to that horrible disease and I went through the motions of living. My fear of the slow disability that would be overtaking me was exacerbated by the grief I felt over losing Avis. Being alone after 35 years of marriage is almost unbearable. She was special and losing her left a very large void in my heart and my life.
I stumbled on in a continually weakening condition until 2000 when I met and married my current wife Robin. I told her about my condition and the fact that there were not enough donor organs for the number of patients who needed them, but she was undaunted and married me anyway. As it turned out she always had more faith than I did that I would get a heart and be just fine, but I was now about five years post diagnosis and my EF had dipped to 20 and I lost another step or two. As I walked the stage in my presentations I started to become more breathless so I contracted my movement circle. It was about this same time when I fainted while driving into a parking place. That development caused my physicians to implant a defibrillator in my chest to guard me against sudden cardiac arrest.
At 9 years my EF was between 15 and 20 and it had become very difficult to be as active as I had been so I made sure that I had a bar stool when I spoke that would be placed about center stage between the lectern and the edge. I could still leave the lectern and give the image of energy but I could kind of lean on that stool. Obviously the heart failure was getting worse, but not bad enough to put me on a transplant list.
Finally at 11 years with an EF of 10 to 15 I quit doing keynote speeches and only accepted small group coaching sessions where I stood on occasion but mostly sat on a stool at the front of the room, and then one day, I couldn’t muster the energy to get through a session unless I sat in a chair.
It was time. We decided to retire and move from Minneapolis, Minnesota to Jacksonville, Florida for two reasons. One being that it was my wife’s  hometown and her family was there and the second was that one of three Mayo Clinics was located there. I learned they had a phenomenal record of success in getting organs and in the survival rates of transplant recipients.
hometown and her family was there and the second was that one of three Mayo Clinics was located there. I learned they had a phenomenal record of success in getting organs and in the survival rates of transplant recipients.
I made the necessary appointments at Mayo and went through a battery of tests for several days. Finally I was told that my case would be presented to the hospital transplant committee for approval to be placed in the national transplant list. Sure enough I was approved and listed and promptly forgot about it. Everything I had read suggested that people on the list waited a long time and that many never got an organ. I was of the belief that at age 68 I was probably too old and not sick enough. After all I was up and around and not even hospitalized.
By now my EF was down to 10 and my heart was getting seriously enlarged. I was on my second implanted defibrillator and had trouble walking from the den to the bathroom without stopping to rest. Then one morning the phone rang, I answered and confirmed my identity and my transplant cardiologist from Mayo said, “I may have a heart for you.”
I could not believe my ears. I had only been listed 13 days earlier.
“Pack a bag and come to the hospital,” Dr. Hosenpud said, “and we’ll get things underway.” In my mind “pack a bag” meant, “Get your butt over here right away, break the speed limit, we’re all waiting for you, hurry, hurry, hurry.”
I told Robin about the call and we rushed out of the house to make the 45 minute cross town drive to Mayo. It only took 30 minutes. For me the world at this point was moving at near the speed of light. My always composed and realistic wife Robin had no delusions. She expected Mayo to be as reserved and professional as they always were. My mind was simply not that organized. I perceived us screeching to a stop at the hospital where a team of the world’s greatest physicians, nurses and technicians would be in  the lobby waiting for us. My mind’s eye saw us running into the hospital surrounded by people in surgical garb and lab coats who were all barking orders while the hospital PA system was calling for more doctors, nurses and technicians. I fully expected the PA system to be saying, “He’s here; the guy who is getting a new heart is here.” I envisioned being thrown on a gurney, stripped of my clothing and rolled at high speed to an operating room where the finest doctors on the planet were assembled next to an ice-covered beating heart in a stainless steel pan.
the lobby waiting for us. My mind’s eye saw us running into the hospital surrounded by people in surgical garb and lab coats who were all barking orders while the hospital PA system was calling for more doctors, nurses and technicians. I fully expected the PA system to be saying, “He’s here; the guy who is getting a new heart is here.” I envisioned being thrown on a gurney, stripped of my clothing and rolled at high speed to an operating room where the finest doctors on the planet were assembled next to an ice-covered beating heart in a stainless steel pan.
T he Doctors looked like Ben Casey Dr. Zorba and Patricia Neal (all stars of the past).The scenario in my mind called for absolute pandemonium. I was
he Doctors looked like Ben Casey Dr. Zorba and Patricia Neal (all stars of the past).The scenario in my mind called for absolute pandemonium. I was  that excited so they must be, too. I needed pandemonium — to have it meant this event was the show of shows, the biggest medical story of the century.
that excited so they must be, too. I needed pandemonium — to have it meant this event was the show of shows, the biggest medical story of the century.
I got anything but. I walked in, stood in a very orderly line and when I was waved forward said to the receptionist, “I’m Bob Aronson and I’ve just been called by Dr. Hosenpud to come in for a heart transplant. “Ok,” I 
 thought. “Cue the marching band and a frenzied atmosphere.” But nothing of the sort happened.
thought. “Cue the marching band and a frenzied atmosphere.” But nothing of the sort happened.
She looked up at me and smiled, looked down at her computer screen and said, “Someone will be out to get you shortly, Mr. Aronson, please have a seat.” There were scores of people in the waiting room and not a single one looked up when I entered. They all sat in perfect silence waiting their turn and ignoring my big event. For all I knew every one of them was here for a transplant as well.
“Have a seat?” I thought. “Don’t they know why I’ m here, who I am? For God’s sake there’s a heart on ice in there beating away, waiting for me and she wants me to sit?” I had considered this day often and each time I did there was pandemonium. I wanted pandemonium, I deserved pandemonium, I needed pandemonium, I craved it, but alas it never happened.
A very nice woman came out in about fifteen minutes and quietly said, “Come with me, Mr. Aronson,” and we slowly, quietly walked behind the reception desk into the surgical area, where I got on a gurney under my own power, put on a gown and was surrounded by very pleasant, highly professional staff who proceeded to quietly and efficiently “prep” me for the surgery.
Finally they wheeled me to a surgical suite where the strains of Beethoven could be heard on the speaker system as the anesthesiologist told me what his role was and about the anesthesia I would be getting. Then, he said he would give me something to “relax” me. It sure did.
I awakened in recovery the next day to the sound of Robin saying, “You have a new heart and you’re doing well.”
Recovery. The Days After
When I awakened again, I didn’t know where I was. I felt like I was duct taped to the bed. My head hurt. I was nauseous and confused. I vaguely remember several doctors entering the room. They asked about pain levels and said they were going to remove my dressings. One of them leaned over me crossed his arms so his right hand was on my right shoulder and his left on my left shoulder, Then there was the sound made by industrial strength Velcro makes when being torn apart rapidly–“Riiiiiiip” and he said, “You Ok?” I don’t remember my response because I lost consciousness again.
They asked about pain levels and said they were going to remove my dressings. One of them leaned over me crossed his arms so his right hand was on my right shoulder and his left on my left shoulder, Then there was the sound made by industrial strength Velcro makes when being torn apart rapidly–“Riiiiiiip” and he said, “You Ok?” I don’t remember my response because I lost consciousness again.
My next awakening was in Cardiac Intensive care. I think I was alone in my own cubicle. There was a nurse there and I was so thirsty my mouth felt like hot sandpaper. I asked for water. The nurse said, “You can have ice chips once an hour and she handed me a glass of them.
They lasted as long as they would had you poured them on a downtown Miami sidewalk at noon in the middle of August and I was still thirsty.  More,” I said.
More,” I said.
“No,” she said, “Not for another hour.”
I begged and pleaded to no avail. So I focused on the wall clock. “57 minutes to go.” It was the longest 57 minutes of my life, but right on schedule she was there with the small glass of ice chips. I was still parched and the chips gave only momentary relief, so I begged again, but failed to penetrate her compassion shield. I think I called her “an ice Nazi.” She didn’t laugh, but it didn’t sway her either. I don’t know how long that went on, but she never relented and I will always remember being the thirstiest I have ever been.
I do not recall how long I was in ICU, but I do remember being moved to my own private room. When I entered the hospital I was suffering from horrible heartburn and I was still bothered by it after surgery so I asked them to place me in the recliner chair in the room. They did and I settled in for the duration. They never cured the heartburn so I never got in bed. I’m probably one of the few transplant patients who spent all my time in the hospital room, some 9 days, without ever getting into bed. The housekeeping staff seemed to like that. One less bed to change.
My Mayo Transplant was done in St. Luke’s Hospital in Jacksonville, Florida while the Mayo hospital was being constructed. St. Luke’s was nice, with an  incredible, wonderful staff, but it was old. In my room there were two chairs, one was the recliner in which I sat. I think it was built in 1915 in Tsarist Russia for use on the enemies of the “Mad Monk” Grigori Rasputin. You had to be a contortionist to adjust the recline angle of the chair and no one who has had their chest cavity carved open has that ability.
incredible, wonderful staff, but it was old. In my room there were two chairs, one was the recliner in which I sat. I think it was built in 1915 in Tsarist Russia for use on the enemies of the “Mad Monk” Grigori Rasputin. You had to be a contortionist to adjust the recline angle of the chair and no one who has had their chest cavity carved open has that ability.
That chair was bad enough, but the other one was clearly meant as an alternative to water boarding. It was a straight backed heavy oak, ladder-back chair. It was designed to make people confess, not to be comfortable and it was what Robin had to sit on, day after day. I don’t know what happened to it since then, but I would bet it is indestructible, probably won’t even burn.
During my stay there, I was constantly wheeled to different tests including heart biopsies, more echograms, X-ray’s and other imaging, pulmonary exams and treatments and meds adjustments. I was weak, still had heartburn, was not eating very much and generally didn’t feel real good, but finally was sent home with instructions on how to recover there.
Post-transplant depression is quite common for a host of reasons, one in particular is guilt. It is not unusual for a transplant recipient to feel terrible because “someone had to die, in order that I could live.” That statement supposes that the organ recipient bears some responsibility for the death of the donor. When you consider it, the thought is unreal and illogical. While I understand that sentiment I respectfully disagree. Here’s my take on the issue. No one HAD to die and when they did, it was not so you could live. That person’s life had ended. They died sadly, because it was their time to go. Prior to that he or she voluntarily signed up to be an organ donor. Then, for whatever reason they died. When they did UNOS (The United Network for Organ Sharing) began a search to look for a match for the organs of the deceased person. You are a number on their list; they don’t have your name.
No one HAD to die so you could get a transplant, but someone did die and you were chosen to get the organ. It’s not as though your donor was called in to the central office and told, “Hey George, today is your turn, We need your heart, kidneys and pancreas. We’ll be putting you down at 3 PM so say your goodbyes.” It just doesn’t work that way. George, for whatever reason, lost his life that day and because he was a generous, compassionate person he had arranged for someone to get his organs upon his passing. Someone, anyone. It is a gift to whoever needs it most. Your donor made that decision, no one else. Be grateful, yes, but guilt has no place in the equation. you are not responsible for your donor’s death.
I seemed to be doing better at home until I awakened one morning with a terrible heaviness in my chest. Breathing was difficult and I was coughing. A call to my transplant coordinator resulted in being instructed to go to the Emergency Room right away. It wasn’t long after I arrived and was examined that I was informed that I had pneumonia and the pulmonologist said he was very worried about my lungs. After nine more days in the hospital and some heavy duty therapy I began to recover and was released.  When I got home I retreated to the den in my favorite recliner, turned on the TV and sunk into terrible depression, a condition that didn’t end soon or easily.
When I got home I retreated to the den in my favorite recliner, turned on the TV and sunk into terrible depression, a condition that didn’t end soon or easily.
Like all transplant patients I was not allowed to drive for a while so at least twice a week Robin had to drive me to Mayo for checkups and treatments. I went because I had to. There was no joy in any of it including the cardiac rehab program, which was well-run, but well beyond my ability to enjoy. This was my lowest point ever. I have since learned that post-transplant depression is very common and yes, I was treated for it, but it is the kind of illness that doesn’t respond immediately to treatment, so I stayed in that state for several months while we experimented with anti-depressants.
At the same time, I was stricken with incredible shoulder, neck, arm and wrist pain. I knew I had the beginnings of osteoarthritis, but I didn’t know it could be this painful. Additionally, I was told that when they perform a heart transplant your arms are placed over your head at a strange angle so the surgeon has complete access to the chest cavity. It is not unusual, I’m told, for some patients to suffer shoulder pain as a result. I was one of those patients. For weeks I suffered from pain so horrible I could not sleep or eat and while the Mayo docs made every effort to help, it took time to find the appropriate method of addressing it. They finally did, but that episode had me descend into even greater depths of depression.
Slowly, very slowly I regained my appetite, my mood brightened and the pain lifted, but it was almost a two year ordeal in which I went from 225 pounds to 150, a 75 pound loss due to having no interest in food and a stomach that wouldn’t keep much down. I think I lived on puddings, gelatins and soft fruits. The only thing that kept me going was a newfound interest called Social Media.
Robin was my salvation in all of this. She not only took care of me at home, but made sure I made all my medical appointments, had the right meds and ran two businesses out of our home at the same time. She is steady as a rock, never panics and is always up-beat and encouraging. Being a caregiver is very hard work. She did it and to some degree still does it without complaint. I am a most fortunate man. I love her with a special intensity and am blessed that she feels the same about me. She is a fantastic woman.

In November of 2007, two months after my transplant I got a call from Lee Aase the social media guru for Mayo Clinic in Rochester, Minnesota. I knew Lee professionally and was flattered when he called to ask if I’d be interested in starting a Facebook group and a blog. I said, “Huh,” and “huh.” I had no idea what either were. Lee is a patient man and took the time to give me a crash course and that’s when today’s over 4,200 member Facebook group Organ transplant Initiative was founded along with Bob’s Newheart blogs. Lee came up with the Newheart name which I still think is mighty clever.
The miracle of the social media for me is that it gave me some new responsibilities, which I desperately needed. My nature is such that if I take on a task I don’t know how to give it anything but my very best. OTI and the Newheart blogs gave me a new reason to get up in the morning. Each day I had something new to do, blogs to write, topics to introduce on Facebook and something to keep my mind off of my miseries. Lee’s call may have saved my sanity.
The Facebook group grew rapidly and the members were incredibly supportive of one another and of me. Since I started blogging I have posted over 260 columns on topics around transplantation/donation and related issues, which is just about any medical story. While some of them were provided by guest bloggers I researched and wrote about 90 percent of them.
Robin is an artist and we sell her colorful anodized aluminum and polymer clay jewelry at art fairs around the east and Midwest and we travel to those s hows with our two dogs in our RV to the tune of about 20,000 miles a year. We love the life, enjoy what we do and have no plans to quit anytime soon.
hows with our two dogs in our RV to the tune of about 20,000 miles a year. We love the life, enjoy what we do and have no plans to quit anytime soon.
Her art business required furnishings for her t ent and because I have always liked doing woodwork I began to build a shop and make shelving, pedestals, picture frames, tables and wooden jewelry boxes. I’m no expert woodworker, but it is a hobby I really enjoy and intend to keep doing it as long as I can. I am busier today than I was when I was working, but now I answer to no one but I and work only on things that give me great satisfaction.
ent and because I have always liked doing woodwork I began to build a shop and make shelving, pedestals, picture frames, tables and wooden jewelry boxes. I’m no expert woodworker, but it is a hobby I really enjoy and intend to keep doing it as long as I can. I am busier today than I was when I was working, but now I answer to no one but I and work only on things that give me great satisfaction.
I am convinced that the road to good health and happiness is made easier if you can stay busy doing things you love doing.
Readers – the only advice I can give you is this. Never give up, never. Be confident of a bright future because if you think otherwise you may be paving your own road to hell. Find something you really like doing, enjoy your new life, love your friends and loved ones with every ounce of your soul and as Spock said, “Live long and prosper.” You’re worth it and you deserve it!
-0-
 Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s over 4,200 member Organ Transplant Initiative (OTI) and the author of most of these donation/transplantation blogs. You may comment in the space provided or email your thoughts to me at bob@baronson.org. And – please spread the word about the immediate need for more organ donors. There is nothing you can do that is of greater importance. If you convince one person to be an organ and tissue donor you may save or positively affect over 60 lives. Some of those lives may be people you know and love. You can register to be a donor at http://www.donatelife.net. It only takes a few minutes. Then, when registered, tell your family about your decision so there is no confusion when the time comes.
Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s over 4,200 member Organ Transplant Initiative (OTI) and the author of most of these donation/transplantation blogs. You may comment in the space provided or email your thoughts to me at bob@baronson.org. And – please spread the word about the immediate need for more organ donors. There is nothing you can do that is of greater importance. If you convince one person to be an organ and tissue donor you may save or positively affect over 60 lives. Some of those lives may be people you know and love. You can register to be a donor at http://www.donatelife.net. It only takes a few minutes. Then, when registered, tell your family about your decision so there is no confusion when the time comes.
The Caregiver — Critical to Transplant Survival
A note from Bob Aronson, founder and publisher of Bob’s Newheart
This blog is a re-print of a piece published by Gift of Life Family House in Philadelphia, Pennsylvania. Gift of Life Family House describes itself as a “home away from home” for transplant patients and their families by providing temporary, affordable lodging and supportive services to those who travel to Philadelphia for transplant-related care. Gift of Life Family House is a 501(c)(3) non-profit charitable organization.
There are many similar organizations at Medical Centers all over the country. Here in Jacksonville, Florida, Gabriel House of Care on the famed Mayo Clinic campus functions much like Gift of Life, but no matter where they are they need outside support with dollars if you have some to spare — and if not, donate packaged goods like paper towels, dish soap and Kleenex that are always in short supply.
In the entire transplant process the daily caregiver is second only in importance to the donor. How important is the caregiver? How important is your life? Most medical centers consider the caregiver of such great importance that if the potential transplant recipient doesn’t have a competent, dependable and compassionate person to fill that role, then he or she may not qualify for a new organ. Have I got your attention?
This post is of equal importance to both the patient and the caregiver. The patient has to be sure he/she not only selects the right person but must ensure that the caregiver has a complete understanding of what the role entails. The caregiver, not only has to understand the role they have accepted but must also make sure the patient understands their capabilities and limitations. Saying, “Yes,” to being a caregiver is making a commitment that is more than taking care of someone for a few days. It could stretch out for years.
Being a caregiver for a transplant patient or recipient is no easy task. It can be emotionally and physically draining and it can also be one of pride and even exuberance but caregivers ought to know what they are agreeing to when asked to take on the job. This advice and information from Gift of Life Family House is invaluable. You can learn more about this organization at http://www.giftoflifefamilyhouse.org/
Transplant Stages for Caregivers
From Diagnosis Until the Rest of our Lives…Organ transplant is a life-long battle. The battle may be very difficult when first diagnosed with a medical issue that requires a transplant but many people feel it becomes easier and is well worth it; however transplant does not end after surgery for the patient or the caregiver. When diagnosed with an illness that will ultimately require an organ transplant some patients and caregivers think that after surgery the battle is over. Having a positive outlook is good but it is also helpful to be prepared for the tough times ahead that can come with a transplant. Caregiver Lifeline will chronicle the stages of transplant and some of the feelings and issues transplant caregivers experience when the patient is initially diagnosed and told they need a transplant; what it is like to wait for a transplant; the actual transplant surgery; what it is like post-surgery up until one year; and lastly, what it may be like post-transplant one year after and on. Some personal accounts of actual transplant caregivers who have been through the stages will also be described in this section.
Diagnosis
Diagnosis of a medical issue that requires a life-saving transplant can produce many different emotions in caregivers and family members. Those emotions can vary from one person to the next and are many times natural feelings that occur when dealing with a difficult medical diagnosis. Regardless of the organ, age or relationship you have with the patient, knowing that your loved one could die without a transplant can be very overwhelming, scary, upsetting and even angering.
At the moment of diagnosis some transplant caregivers and family members have admitted that they were very scared, but quite often due to lack of information and education about what their loved one was going through and what to expect in the future. Once they received that information their feelings of being scared or upset decreased because they knew what to expect. One brother of a kidney recipient admitted feeling very scared when he and his family initially found out about his brother’s kidney disease. He then described feeling more confident once he learned more about his brother’s condition and even better when he found out he could donate his own kidney to his brother, which he eventually did. The education this family received helped them prepare for the future and cope better with their situation. Not all individuals and families are alike. Other families and patients have admitted that too much information is a bad thing for them and they become more anxious or scared when they are given too much information all at once. It is helpful to know what type of person you are: do you like all of the information “no holds barred” or a little information at a time so you have time to process it at your own pace? Letting the transplant team know how you and your family would like to be treated can be very helpful so they can try to treat you and the patient accordingly.
When the diagnosis of an illness that requires a transplant happens suddenly, families and caregivers can be overwhelmed and may not retain information given or may forget to ask important questions about the transplant process. Some questions that may be helpful to ask the medical team are:
- Why does the patient need a transplant?
- Who will the patient receive a transplant from?
- How long will the patient need to wait for a transplant?
- What other treatments options are available?
- What treatment will the patient need to receive while they wait for their transplant? And how will that treatment affect their life (will they need to stop working, or will they need to be hospitalized?)
- Will the transplant prolong their life?
- What will be required after they receive a transplant? More hospitalization? Medication?
- How much will everything cost? And what will happen if we can’t afford the cost?
It is helpful to keep these questions and answers written in a journal to have available to look on when needed.
One mother describes finding out during her pregnancy that her son had significant kidney issues while in her uterus and he may not survive. She described being very shocked after already having given birth almost two years previous to a healthy son. She also described feeling like she was in a “nightmare waiting to wake up.” She states she never woke up and had to come to the realization that their family was in for a tough ride, if her son survived at all. Fortunately her son did survive and he was eventually able to receive a kidney transplant.
Many people who require a transplant have some knowledge beforehand that a transplant may be necessary. For instance, one transplant caregiver of her son (who required a heart transplant) was somewhat prepared for the day they were told he would need a new heart. Her son had medical issues for many years and a transplant was always a distinct possibility. During the time previous to needing a transplant this mother had a chance to educate herself on the process so the initial diagnosis was not a huge shock or completely overwhelming. This mother was still scared due to the risk of surgery and the risk the new heart would not work, but she also had a chance to become prepared and ask for support from her family and friends.
It may be difficult to prepare for a diagnosis that you had no previous knowledge of or any reason to prepare for, which is why it is ok to call your transplant team at any time if you have a concern or question. You could also make an appointment after you compile all your questions together. It seems scary to go home from the hospital or the doctors not having all the information you would like, so you can always perform the research yourself through reputable internet sites like www.Donors1.org or www.UNOS.org. The next step in the transplant process may also allow for some extra time to prepare for the future.
The “Wait”
Between the time when a patient, caregiver and family receive the news of needing a transplant and when they officially have surgery and receive their new organ, there is a waiting process. The wait while the patient is actually on the UNOS wait list can be short or very long, though there may be many emotional and physical issues experienced by the patient and family regardless of the duration of their wait. Quite a few things can determine how quickly a person receives a transplant and those standards differ from one organ to the next. For instance, a kidney transplant could happen rather quickly if a patient has a family or friend who is willing to be their living donor. A willing person (not bribed or forced) must be tested to see if they are a match for the patient. If they are a match, surgery can be scheduled and the transfer of kidney from the living donor to the patient can happen. If a person has no willing, matching, living person to donate to them, then they are placed on a waiting list through UNOS and must wait for a kidney from a deceased donor.
Some hospitals also do living donor liver transplants, where a willing person can donate part of their liver. The living donor must also match the recipient, though the guidelines are different than are for a living kidney donor transplant. Heart, lung and pancreas are organs that must be taken from a deceased donor, which unfortunately may make the wait longer. For more information on the specifics of different organs and wait times please visit the UNOS Website.
Because the wait time is so unknown, many caregivers and patients feel out of control and powerless. One mother described how helpless she felt and that there was nothing she could do to help her son while he was waiting for a transplant, which caused her much stress. Many caregivers and patients experience emotional “ups and downs” while waiting for a transplant because the future is unknown. It is not uncommon to feel like you are living one day to the next hoping for the call from the transplant center about a possible organ for your loved one. A transplant social worker suggested that one way to feel more in control during the wait time is to stay in contact with the transplant team, call when you have questions, keep appointments as scheduled and help the patient take responsibility for their health care. By staying in contact with the transplant team, you and the patient can feel more connected to the transplant process which may alleviate some of the uncertainties of the wait process.
During the wait process caregivers experience many different emotions. One of the most common emotions described by caregivers is fear that their family or friend will not live long enough to get their organ. Others experience emotions such as anger at the patient, medical team, or even themselves. Some caregivers may feel anxiety regarding their own life regarding their financial situation and how they will afford to care for their family member or friend and whether they will have to stop working or stop doing things they enjoy. Another emotion may be denial. Caregivers may think the issue is not as serious as it truly may be. Most emotions felt by caregivers are natural and quite universal. Support groups can be very helpful because it allows transplant caregivers to hear some of the universal concerns and issues of other transplant patients and caregivers. It is also common for a caregiver to feel as though they are the only person on earth going through the issues related to being a transplant caregiver, which is another reason a support group can be helpful. It can be beneficial to be able to talk to others who have dealt with or are dealing with the same issues.
Another emotion that many patients and families feel is grief; some even call it “survivor’s guilt.” One mother described feeling quite a bit of grief that she was waiting for someone else to die in order for her son to receive a kidney to live. She states, “That was the hardest part for me, knowing that our overwhelming joy would be another family’s overwhelming grief.” A different mother to a 14 year-old heart recipient was so excited when her son received his heart and had a second chance at life, but her family struggled for some time as well realizing that another person passed away in order for her son to receive a heart. She stated, “We are so joyful that our son will have a second chance but it is tempered because there is a huge loss associated with it for someone else.” This type of feeling is extremely natural for many transplant caregivers and organ recipients. In the exception of a living kidney or liver donor, in order for one person to receive an organ transplant, another person will pass away and their family has the option to donate their organs. However it is a wonderful gift for a person to donate their organs after they pass away, because it is giving another person a second chance at life. To understand the donation process better, visit www.Unos.org or www.Donors1.org.
The wait for an organ can vary so it may be helpful to address your feelings as they occur and get help if you are in need. Finding out that others have gone through similar issues can be helpful through support groups. Talking to the transplant social worker can also be beneficial because they can connect you to other options such as counseling or other supportive services. Support groups and counseling can be helpful to the patient as well as the caregiver because the wait process can be difficult for both parties. Don’t forget to include other siblings or family of the patient because many times they may also have similar feelings requiring additional support.
During the waiting period, caregivers and family may have time to prepare for the future. Finances usually play a large role in any medical issue that requires a lot of medication or frequent appointments or hospitalization. Because transplants are not over after surgery, planning and preparing for the financial cost is important. There are many resources to assist with transplant costs if a person has limited means. For instance, most prescription companies provide assistance for drug costs. Many large hospitals also may have financial assistance programs for patients. If there is ever a financial concern, talk to the transplant social worker immediately and let them help through the process. Many times the caregiver is left to deal with those issues, especially if they become the financial provider because the patient cannot work. As the caregiver your employment may become affected, which could also affect your health insurance. It may be helpful to prepare your employer if there is going to be any changes with your ability to work and how that could affect your health insurance.
Also see Financial Burden on Caregivers for more information.
In addition to planning financially or preparing for your own work issues, it may be helpful to begin to talk with the patient about their future. The patient’s future can include many different things, so it is important to identify what is important to them. For instance, has the patient thought about their job or hobbies and how that will affect their financial state or health insurance? It may be scary to think about, but what if the patient becomes too sick and no longer can make decisions? Who will be the medical power of attorney or a financial power of attorney? Does the patient have an advance directive, and if not, do you know their wishes? Your relationship with the patient may determine your involvement in their care if they cannot make their own decisions, however it is still important to encourage the patient to think about their own future.
Transplant Surgery
Finally, your family member is getting their organ and a second chance at life! Transplant surgery can be very exciting because the wait is over and life can restart. You may be able to go back to work or begin doing what you used to enjoy; the patient can be normal again, and live a long, happy, healthy life. All of this can be true but the surgery and recovery are very important and sometimes the most difficult part of the transplant process.
During the transplant surgery stage the patient can be hospitalized for anywhere between 5 days and 14 days, without complications. If there is a complication during surgery the patient may then be required to stay in the hospital for longer than expected. At this time you may physically not want to leave the patient’s side but you may also have to take care of the rest of your family or continue to work. It can be very stressful for a caregiver to balance their life with that of the patient’s transplant recovery. It is important for a caregiver to remember that taking personal time is essential, even during this time, because chronic stress can build up and potentially cause medical and emotional issues which could limit the caregiver’s ability to be a good caregiver. Leaving the hospital for an hour a day, or taking an hour a day to do something enjoyable could make a positive difference while dealing with the stress involved with the hospitalization. Don’t forget there are many transplant team members available if you have any concerns.
Post Surgery – 1 year
Many transplant social workers have said that the first year after a transplant can be very difficult for patients and families. Transplant does not end after surgery, and many times people feel that after surgery and a short recovery everything will be fine and life will resume with little obstacles. Sometimes it is not always possible to jump back into your previous routine and lifestyle so quickly. For some people, one year after transplant can be the most difficult. Trying to get your life back while the patient is continually being monitored by doctors for rejection and getting used to a new life with a new organ can be tough. Each organ is different and recovery times and needs are different for each patient, so it is important to always talk to the transplant team about concerns or questions and to better understand what it could be like for the patient.
One family stated they were in and out of the hospital more in the one year post-transplant than any other time because of so many rejection episodes. Every patient and transplant is different; some patients experience many rejection episodes and need to go back and forth to the hospital, which is not uncommon, while other patients may never experience a rejection episode. If the patient feels they are having symptoms of rejection, it is important to follow the discharge directions from the transplant team and contact them as soon as possible.
Because recovery times can differ from one transplant to the next it is not easy to identify a set recovery time. For lung transplants, a patient may be required to attend up to three appointments per week post-transplant for up to three months, whereas for a kidney transplant only two appointments for 6 weeks may be required. If a person does not reside in the transplant hospital area it can make life even more difficult post-transplant. Similarly, if the caregiver needs to return to their life or work they also may have a tough time arranging the patient’s transportation to and from the hospital for their appointments. It may seem stressful for a transplant caregiver one year post-transplant because there may be alot of pressure to keep the patient healthy with their new organ. Some things that are important to consider after transplant is monitoring for rejection, getting used to taking new medications, nutrition, getting back to doing things you and the patient love and keeping a positive outlook. Talk to your transplant team to find out the best way to monitor the patient post-transplant, as every patient is different.
Depression and other mental health disorders have been known to be prevalent up to one year post transplant, and emotional health could affect compliance which can in turn affect the survival of the transplant. Caregivers may also experience symptoms of depression due to lifestyle changes and stress that transplant can cause. Caregiver and family support has been found to be very effective in assisting with emotional and mental issues post-transplant so the caregiver should always plan for continued contact with the medical team as needed.
As a caregiver it can be an emotional rollercoaster trying to monitor the patient’s health after a transplant while living your own life and caring for other family members or working. The section about compliance may provide some assistance when it comes to getting the patient to care for their organ and prevent rejection with good compliance. The transplant team is there to help with concerns and issues as well. Please see Emotional Health for Transplant Caregivers for more information.
Post Transplant – Until the Rest of our Lives
The patient will always have their transplant doctors and team to contact with questions or concerns at any point down the line. Transplant is life-long and although stable patients’ and families’ contact with the transplant team may lessen, the transplant team should always be there for the patient and family as long as needed.
At this point in the transplant the patient may be stable enough to have very little contact with the transplant team; therefore it’s time to get back to life if you and the patient have not done so already. It is recommended to go back to enjoying things you and your loved ones once enjoyed. One important reason a person would want to receive a transplant would be to extend their life so they can continue to live their life by doing what they love.
Many caregivers have a difficult time letting their caregiver role go because it has been an identity for quite some time. If there is no need for you to be a caregiver any longer then it is important to move on to your next role and place the caregiver role on the back burner. If you enjoyed being a mom, a worker or soccer coach for example, then take on those roles again and make them an important priority. The same can be said for the patient who may no longer be the patient, and also must place that role to the side. This stage can be difficult for both parties because many people have trouble returning to work, or spending time with friends without having a constant worry of the transplant patient.
How can a caregiver stop being a caregiver? It may be helpful to first identify what you enjoy in life. Do you love being a mother? Did/do you love your job? Did you previously spend every Thursday with your friends playing golf or going to the movies? Then try to do those enjoyable things as often as possible without thinking about transplant. Encourage the patient to do this as well.
Though you are being encouraged to let the caregiver role go, it does not mean you and the patient no longer have transplant responsibilities. Transplant is a lifelong process so you and the patient may need to take on the patient/caregiver role again at some point down the line. Additionally, there are some transplant pieces the patient cannot put on the back burner, such as good nutrition, exercise and medication compliance.
Another piece of life post-transplant is you and the patient continuing to live a healthy lifestyle. The patient will need to keep their new organ healthy, and as a caregiver you may play a large role in encouraging them. Without good health the organ could reject, placing the patient back where they were previously: needing a transplant. The patient’s transplant team, including their dietician, will be able to give good advice on good nutrition and exercise for the patient. Similarly, it is important for you to have good nutrition and exercise practices to keep yourself healthy as well. Good nutrition and exercise habits have even been shown to decrease depression. Please see the Physical Health for Transplant Caregivers and Emotional Health for Transplant Caregivers sections for more information and education for the caregiver.
Don’t forget to live your life to the fullest now that you and the patient have a second chance at life. The transplant is giving you and your family the opportunity to appreciate life and everything it has to offer.
-0-
Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s nearly 2,500 member Organ Transplant Initiative and the author of most of these donation/transplantation blogs.
You may comment in the space provided or email your thoughts to me at bob@baronson.org. And – please spread the word about the immediate need for more organ donors. There is nothing you can do that is of greater importance. If you convince one person to be an organ and tissue donor you may save or positively affect over 60 lives. Some of those lives may be people you know and love.
Please view our video “Thank You From the Bottom of my Donor’s heart” on http://www.organti.org This video was produced to promote organ donation so it is free and no permission is needed for its use.
If you want to spread the word personally about organ donation, we have another PowerPoint slide show for your use free and without permission. Just go to http://www.organti.org and click on “Life Pass It On” on the left side of the screen and then just follow the directions. This is NOT a stand-alone show; it needs a presenter but is professionally produced and factually sound. If you decide to use the show I will send you a free copy of my e-book, “How to Get a Standing “O” that will help you with presentation skills. Just write to bob@baronson.org and usually you will get a copy the same day.
Also…there is more information on this blog site about other donation/transplantation issues. Additionally we would love to have you join our Facebook group, Organ Transplant Initiative The more members we get the greater our clout with decision makers.
Transplants — With An Emphasis on Recovery (by organ)
The organs most commonly transplanted are Heart, Kidneys, Liver, Pancreas, Lungs and Intestines. The entire process of organ transplantation is traumatic, from the time you are diagnosed through the evaluation process, your time on the waiting list and finally recovery from the surgery. If you are told you are going to need an organ transplant you are also being told that your life is about to change dramatically.
THE DIAGNOSIS
When you are diagnosed as needing a transplant you are being told that there are no good recovery alternatives for your disease. It is likely that most of them have been tried. While the physician is unlikely to tell you that your days are numbered you will probably hear that you that you have an end-stage disease. That’s Dr. talk for, “You are dying.” Getting that news is a traumatic event and you may need to discuss it with someone or even get professional help.
In order for your medical team to determine if you need a transplant you will have to undergo a thorough physical and mental evaluation. Before they do that, though, there is a critical questions that must be answered, “Do you have the financial resources to pay for a transplant should they find that you need one?” If you cannot answer that question affirmatively a hospital social worker might be able to help but your chances of getting a transplant will be delayed until that single question gets a positive answer. Once answered, though, the evaluation process begins and you will embark on an unprecedented medical voyage. Among other things they have to determine that you are a good surgical risk.
In addition to assessing your physical condition, the team will consider your attitude and psychological state among other factors. Donated organs are a rare commodity, so doctors don’t want to proceed unless they are sure that a patient is physically and mentally prepared for both the procedure and for life following it. Your transplant team will also want to ensure that you have a competent caregiver, someone you can depend on to watch over your recovery. This is a key element of the process, you simply must be able to show that you have a caregiver who will make a significant investment of time as you regain your strength so you can return to a “normal” life.
And…a caution if you smoke or are addicted to either drugs or alcohol chances are you will be told you must quit or there will be no transplant. Generally you have to show that you have abstained from the two for at least six months. Again, organs are precious and there aren’t very many available so medical facilities want transplant candidates that can prove they will take good care of them.
When the tests are complete and show clear medical evidence that you need an organ transplant, your physician will present your case to the medical center transplant committee. If they approve, you will be added to the national transplant list at the United Network for Organ sharing (UNOS). Then the wait begins and that, too, is traumatic. Some people never get an organ, others wait a long time and some, like me are luckier and have a short wait. Mine was only thirteen days but it took twelve years after my diagnosis before I was sick enough to get on the list.
THE SURGERY
Once the transplant committee approves you for the procedure you will be placed on the national transplant list and then you wait…you wait for “THE CALL.” When it comes you will be asked to get to your medical center rather quickly where they likely will perform additional tests in preparation for the surgery. Prep includes giving you something that will “relax” you. In reality it will knock you out.
You will awaken in intensive care, surrounded by beeping, chirping monitors, IV bags hanging from chrome stands, electrodes attached to your body and perhaps a ventilator. Awakening from the surgery can be scary, because you may not be fully aware of what happened or where you are, and because of the ventilator you will be unable to talk. Most often they remove the “vent” as soon as possible. In my case it was gone when I awakened.
Usually the medical staff will try to get you on your feet and moving around as soon as possible but depending on the transplant and your condition hospital stays can range from a week or so to a much longer period of time. Then there is the recovery process and having gone through it this blogger strongly advises you to do everything your physicians suggest because that’s what will keep you alive.
As I mentioned earlier, the organs most commonly transplanted are Heart, Kidneys, Liver, Pancreas, Lungs and Intestines. Recovery from these surgeries is sometimes difficult and for a while following surgery you will make many return trips to see your coordinator and physician.
THE RECOVERY
Critical Information You Need To know
Below I have listed the recovery process for all six of the organ transplants I listed earlier. I chose to use a different transplant center for each organ to show that while centers may differ a little in the recovery process the bottom line is always the same and that is to ensure that the patient has a sound recovery and can then lead a healthy and satisfying life.
Kidney Transplant Recovery
Cleveland Clinic
Frequently Asked Questions
Now that I feel better, when can I return to my regular activities?
You can resume your previous activities as soon as you feel better — and you might even feel good enough to add some new activities. A daily exercise program will continue to improve your health and help you maintain a positive attitude.
You will not injure yourself or your new kidney if you follow some of these general guidelines:
- Avoid lifting heavy objects and strenuous physical work for at least six to eight weeks following surgery. It is important that you also do not lift anything heavier than 20 pounds for two to three months, and nothing heavier than 40 pounds for four to six months from the date of your surgery.
- Avoid driving for at least six weeks following surgery. Plan ahead so a friend or family member can help out during this time. When you are in a moving vehicle, always use your seat belt.
- Exercise is encouraged, and we recommend beginning with stretching exercises and walking. Other excellent exercises include jogging, hiking, bicycling, tennis, golf, swimming, and aerobics. All of these can help you regain your strength and may be started gradually after your incision has healed.
- As a general rule, rough contact sports should be avoided since they might cause injury to your transplanted kidney. If you have doubts about any activity, please ask the Transplant Team.
When will I be able to return to work?
Many kidney transplant patients are able to return to work within a few months following a successful surgery. However, various aspects of the recovery process can effect the timing of your return.
You will need to discuss returning to your job with the Transplant Team. When the time approaches, a “return to work” letter will provided. This will let your employer know when you may begin working and what limitations, if any, you have.
How soon can I take a vacation?
You may travel as soon as you are feeling better, but always let the Transplant Team know when you plan to go and provide a phone number where you can be reached. By remembering these traveling tips, your vacation will be worry free:
- Always take all of your medicine with you and make sure you have enough medicine to last throughout your trip.
- If you are traveling by plane, carry your medicine with you. Never check them with your luggage.
- Make sure you have your Transplant Center’s phone number.
- Check to see if there is a medical laboratory or transplant center nearby where you can have your blood work completed. This lab will need to report your results to your Transplant office.
Heart Transplant Recovery
Mayo Clinic
Because I got a heart transplant at the Mayo Clinic in Jacksonville Florida in 2007 it is the one with which I am most familiar. I was in the hospital for 9 days and experienced little discomfort other than feeling weak.
What you can expect
During the procedure
Heart transplant surgery usually takes about four hours — longer if you’ve had previous heart surgeries or if there are complications during the procedure. The surgeon will open your chest and connect you to a heart-lung machine to keep oxygen-rich blood flowing throughout your body. The diseased heart is removed, and the donor heart is sewn into place. The new heart often starts beating when blood flow is restored. Sometimes an electric shock is needed to make the donor heart beat properly.
You’ll be in pain after the surgery, which will be treated with medications. You’ll also have a ventilator to help you breathe and tubes in your chest to drain fluids from around your lungs and heart.
After the procedure
After you’ve had surgery to place your donor heart, you’ll likely remain in the hospital for a week or two, and then you’ll be closely monitored at your outpatient transplant center for about three months. While at the transplant center, you’ll have regular tests on your donor heart, including blood work, echocardiograms, electrocardiograms and heart biopsies.
There are also several long-term adjustments you’ll need to make after you’ve had your heart transplant. These include:
- Taking immunosuppressants. These medications decrease the activity of your immune system to prevent it from attacking your donated heart. Because your immune system will most likely never get used to the new organ, you’ll take some of these medications for the rest of your life.
These medications may cause noticeable side effects. With taking some post-transplant drugs, such as corticosteroids, your face may become round and full, and you may gain weight, develop acne or facial hair, or experience stomach problems. Some of the effects are more noticeable when you first start the drug regimen, but decrease in severity later on.
Because immunosuppressants make your body more vulnerable to infection, your doctor may also prescribe antibacterial, antiviral and antifungal medications. Some drugs could worsen — or raise your risk of developing — conditions such as high blood pressure, high cholesterol, cancer or diabetes. Over time as the risk of rejection is reduced, the doses and number of anti-rejection drugs can be reduced, but you will need some immunosuppressant medications indefinitely.
- Managing medications and therapies. After a heart transplant, taking all your medications as your doctor instructs is important. It’s a good idea to set up a daily routine for taking your medications so that you won’t forget. Keep a list of all your medications with you at all times in case you need emergency medical attention, and tell all your doctors each time you’re prescribed a new medicine.
- Cardiac rehabilitation. After your transplant, you may find it difficult to adjust to new lifestyle changes, such as diet and exercise. Cardiac rehabilitation programs can help you adjust to these changes so that you can regain your strength and improve your quality of life.
- Emotional support. Your new medical therapies and the stress of having a heart transplant may make you feel overwhelmed. Many people who have had a heart transplant feel this way. Talk to your doctor if you’re feeling stressed or overwhelmed. Transplant centers often have support groups and other resources to help you manage your condition.
Lung transplant Recovery
Duke University Medical Center
Use these patient resources to understand steps you need to take after your lung transplant procedure at Duke. Click on the links for full details.
Infections in a transplant patient can be quite serious, even life-threatening. Good hand washing, along with a few other practices will help prevent infection.
After lung transplant, your health will be constantly monitored to ensure that your lungs are healthy and not being rejected .
Learn what symptoms may signal infection and find out what steps to take to maintain your health and prevent infection.
After transplant, your body is more susceptible to infection. Learn how to avoid and manage common infections.
Rejection of your transplanted lung(s) can occur at any time following your surgery. Discover steps to take to avoid rejection or ways to manage your health if you do experience rejection of your new lungs.
Learn what to expect in regards to pulmonary preparation and rehabilitation before and after lung transplant.
Diet and nutrition are very important aspects of everyday care after a lung transplant. Find guidelines to keep you healthy after transplant.
Sexual activity doesn’t have to be avoided after lung transplant. Following a few simple guidelines will ensure that you stay healthy while enjoying sex.
When patients show signs that their new lungs are being rejected, we have a number of ways to combat that rejection including steroids, RATG, and Campath.
Pancreas Transplant Recovery
Vanderbilt University Medical Center
You will be encouraged to get out of bed as soon as possible– usually the first or second day after surgery. This is an important way to prevent pneumonia. We will encourage you to walk around your room and down the hall at least three times a day. Walking increases your blood circulation, helps relieve gas pains, and helps maintain your muscle tone.
Each morning, we will draw blood to follow your progress and adjust your daily medicines. The most important blood tests to measure your kidney function are B.U.N. and CREATININE.
Another way to watch your new kidney’s progress is to accurately measure how much fluid you drink each day and how much urine you put out. At first the nurses will measure this for you. Eventually you will be taught to do this for yourself.
You will be weighed daily before breakfast. It is important to weigh at the same time each day on the same scales with the same clothes on. This is a habit you’ll need to continue after you’re sent home. Weight gain can be a sign of rejection of your new kidney.
Once you and your nurse feel you are able to care for yourself outside the hospital you will be sent home. If you live out of town you may want to stay at the Guest House Inn near Vanderbilt for a short period of time after discharge. During this time you will be coming back to Vanderbilt for outpatient evaluation two to three times per week.
Liver Transplant Recovery
University of California San Francisco
After surgery, you will go directly to the intensive care unit (ICU), usually for one or two days. Immediately after surgery, a breathing tube will be inserted to help you breathe. In most cases the tube can be removed within 24 hours after surgery. Many monitoring lines also will be attached; these, too, will be removed as you become more stable. When you are ready to leave the ICU, you will be cared for on the 14th floor of the hospital if you’re an adult. Children are cared for on the sixth or seventh floor. Everyone recuperates from liver transplantation differently. Depending on your condition, you will be hospitalized for two to eight weeks following the transplant.
After the Hospital
After you are discharged from the hospital, you will be seen in the liver transplant clinic at least once a week for the first month. As you improve, you will be seen less often; eventually, you will be seen once a year.
If you are not from the San Francisco area, you probably will need to stay close by for the first month after discharge. After that, your doctor or a specialist near your home will provide follow-up care. Laboratory blood tests are obtained twice a week following transplantation. Gradually, the frequency of blood tests will be reduced.
You will be notified about any adjustments in your medications. Complications can occur with any surgery. Patients undergoing organ transplantation may face additional complications. The life-threatening disease that created the need for your transplant may affect the functioning of other body systems. Other risks, such as rejection, also may occur.
Some possible transplant complications and medication side effects include:
- Hemorrhage — One function of the liver is to manufacture clotting factors. When a liver fails, the ability to produce clotting factors is impaired. To correct this problem, you will receive blood products before and after surgery. It is expected that your new liver will start working very quickly to help prevent any excessive bleeding, but it is possible that you may be returned to surgery to control the bleeding, particularly if it occurs within the first 48 hours after transplant.
- Thrombosis — This is a serious complication that may require a second transplant. If a blood clot forms in a vessel leading to or from your liver, this may injure your new liver. You will receive special anticoagulation medication to prevent thrombosis.
- Rejection — Your body’s defense system, the immune system, protects you from invading organisms. Unfortunately, it also views your new liver as foreign and will try to destroy it in an attempt to protect you. This is known as rejection. To prevent this from occurring, you will be given special immunosuppressive medication that must be taken for the rest of your life. Rejection can be diagnosed early by performing weekly liver biopsies during the first few weeks after liver transplant. Although rejection is common, with early diagnosis and treatment the situation can be controlled in more than 95 percent of cases.
- Recurrent disease — Many liver diseases may come back after your transplant. Hepatitis C is the most common disease that can reoccur following a liver transplant. Your doctors will discuss this further with you.
Intestinal Transplant Recovery
Georgetown University Medical Center
The Healing Process
After your small bowel transplantation, there are two challenges. First, you must manage the pain and recover. Second, you must learn to manage living and eating with a transplanted small bowel.
Will I be in pain?
Immediately following surgery, you will experience pain. We will do everything we can to make you as comfortable as possible. Most transplant patients have a significant reduction in pain several weeks after surgery. Some people continue to have some discomfort for a longer time.
Where will I spend my time in the hospital?
Immediately after surgery, you will be transferred to the intensive care unit. You will spend several days there as the Transplant Team monitors you very carefully.
After your stay in the intensive care unit, you will be transferred to the General Transplant Unit, where you will be instructed on how to assume responsibility for your everyday care. You will be encouraged to get out of bed at least three times a day and walk around your room and the halls. This increases your circulation and aids in healing.
What are the possible risks and complications?
You team is watching for the following possible complications:
- Increased ostomy output
- Fever
- Nausea and/or vomiting
- Blood in stools/ostomy output
- Change in appetite
Please do not be scared or anxious about possible complications. Our team has many solutions for possible complications. All transplants carry risk and we will do everything we can to minimize those risks.
How long will it take to know if the new small bowel is working?
There may be a delay in the function of your transplanted small bowel. This may increase the length of your stay in the hospital as well as the risk of complications. There is also the possibility your transplanted small bowel will not function. You would be relisted in the highest priority category allowed.
What about the possible risk of infection?
Infection is always a concern following any major surgery. The Transplant Team will monitor you for signs and symptoms of an infection.
How long before I can leave the hospital?
You must remain in the local area (within two to three hours of Washington, DC) for four to six weeks post discharge for monitoring
While the information you just consumed is general in nature you will likely find that with a few modifications it is the process most transplant centers will follow. If you have more specific information needs you should call your transplant coordinator, social worker or physician.
Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s nearly 2,500 member Organ Transplant Initiative and the author of most of these donation/transplantation blogs.
You may comment in the space provided or email your thoughts to me at bob@baronson.org. And – please spread the word about the immediate need for more organ donors. There is nothing you can do that is of greater importance. If you convince one person to be an organ and tissue donor you may save or positively affect over 60 lives. Some of those lives may be people you know and love.
Please view our video “Thank You From the Bottom of my Donor’s heart” on http://www.organti.org This video was produced to promote organ donation so it is free and no permission is needed for its use.
If you want to spread the word personally about organ donation, we have another PowerPoint slide show for your use free and without permission. Just go to http://www.organti.org and click on “Life Pass It On” on the left side of the screen and then just follow the directions. This is NOT a stand-alone show; it needs a presenter but is professionally produced and factually sound. If you decide to use the show I will send you a free copy of my e-book, “How to Get a Standing “O” that will help you with presentation skills. Just write to bob@baronson.org and usually you will get a copy the same day.
Also…there is more information on this blog site about other donation/transplantation issues. Additionally we would love to have you join our Facebook group, Organ Transplant Initiative The more members we get the greater our clout with decision makers.
“His” Heart, My Life, My Story
I wrote this account of my life since receiving a heart transplant in hopes that others will benefit from my experiences. Most of you who will have transplants will have a far easier time of it than I did. You must remember that I was 68 years old when I had mine and that alone can make a huge difference in recovery time and other factors as well. If any of you have any questions after reading this please contact me personally at bob@baronson.org.
Being a transplant recipient is an amazing experience. I simply cannot describe what the feeling is like knowing that one of the parts you were born has been discarded and replaced with one belonging to someone else who in all likelihood died…except for the organ that is keeping you alive.
I don’t know who my donor was. I only know he was about 30 years old when he died and he was from South Carolina. I have written to my donor family but not heard from them so I assume they prefer to remain anonymous and I understand and accept that.
Everyone who has ever had a transplant has had a unique experience that nothing else in life can match. Each day I am struck by the awareness that the heart I was born with, that kept me alive for 68 years no longer beats within my chest. It died. I didn’t. Wow!
Often when I lie in bed I feel the rhythmic thumping that kept someone else alive for 30 years is now doing the same for me. “His” heart is my life. “His” heart pumps my blood, in my body to my brain and allows me to think, to live, love and enjoy life. “His” heart, not mine.
My donor has given me a lot but his greatest gift is allowing me the extra time to be with my wonderful wife Robin.
In 1995 after collapsing in a parking ramp am rushed to a hospital, I was diagnosed with dilated idiopathic cardiomyopathy and was told that someday I might need a heart transplant. As the owner of a communications consulting business I was very active and travelled a great deal both domestically and internationally, but slowly my health began to deteriorate. Always the optimist I adjusted and slowed down a little but not so anyone would really notice.
Then in 1996 my wife was diagnosed with lung cancer and I ignored my condition while we dealt with hers which included many chemotherapy and radiation sessions. After a long and courageous battle with that terrible disease she succumbed in November of 1998. We had been married for 35 years. It was a devastating time and at age 59 I felt lost, alone and without hope as I began to feel the effects of my own condition.
About a year later I met Robin Diffie and as we got to know each other I felt my life just might come back together after all, but my version of the sword of Damocles, cardiomyopathy, continued its swing through my life as my heart function continued to fall with a resultant decrease in my ability to function.
In 2000 Robin and I were married in Eagan, Minnesota but by then the condition which would later require a heart transplant was becoming debilitating, when I travelled I began to ask for wheelchair service in airports and Robin began traveling with me to make sure I got one and to act as my “pusher.”
Cardiomyopathy kind of sneaks up on you and kicks your butt softly at first but then harder and harder. The effect of the disease is measured by ones “Ejection Fraction” (EF). A normal heart will pump out about 60% of the blood it contains every time it beats. As the disease progresses the EF keeps going down and the heart enlarges in order to store the blood that doesn’t’ get ejected. My heart was getting very large and by 2006 my EF was around 10% and decreasing. Clearly I was dying and too sick to work. Sometimes I could barely walk a few feet without having to stop to rest. My heart was just barely pumping enough blood to keep me alive. Reluctantly I made the decision to retire.
It was then that we decided to move to Jacksonville, Florida and we did so for two reasons. 1) Moving there offered the greatest likelihood of getting a heart. My research indicated that the Mayo Clinic in Jacksonville had a wonderful record in organ procurement and transplantation. 2) It was an easy decision because Jacksonville is Robin’s home town and her entire family is there. I still question Robin’s sanity in marrying a dying man but no matter I am grateful for whatever bug struck her and caused the instability.
After undergoing the battery of tests that are required to qualify for a transplant, I was finally approved and placed on the national list on August 8th of 2007. I had resigned myself to either a very long wait or, I thought, no heart at all because of my age. It had already been twelve very long years since I was diagnosed with a fatal heart disease. I thought that at age 68 it was unlikely that I would get a heart and if I did it wouldn’t be anytime soon — but I got lucky.
Only 13 days after being listed I got the call from Mayo Clinic Transplant Cardiologist Dr. Jeffrey Hosenpud that he “might” have a heart for me. He did. I got one and August 21st 2007 goes down in history as my “other” birthday.
My recovery from the transplant was difficult to say the least. It took four years before I finally felt good again. I quit smoking in 1991 but the 37 year habit had already taken its toll, I had Chronic Obstructive Pulmonary Disease (COPD). That’s a disease of the lungs that can best be described as feeling as though you are breathing through a straw…try that some time. COPD is bad enough but when you get pneumonia on top of it you have another life threatening situation. Well, I got pneumonia shortly after my surgery and was hospitalized again but the recovery was very slow and touch and go before I slowly regained my strength. I now know that another bout with pneumonia could kill me so I try to be pretty careful about what I expose myself to.
I no sooner recovered from the pneumonia virus than I was stricken with indescribable absolutely excruciating pain….pain so severe that sometimes I would just sit and cry. Part of the pain, I’m told, was the result of the way I was positioned during my surgery. Apparently your left arm is in a strange position in order to allow the surgeon unobstructed access to the chest cavity, but a transplant takes a long time and it seems that my arm needed different medical attention than was delivered.
The pain in my left arm right down to my wrist and fingers was awful but then just when I thought it couldn’t get worse, it did. The pain spread to both shoulders, my neck and lower back for and went on for months. Torn rotator cuffs were part of the reason but much of the pain came from unknown causes, perhaps it was the way I was sleeping or maybe the lack of proper exercise and maybe because of an old auto accident. We’ll never know the exact cause but it was finally resolved with a combination of physical therapy and Oxycontin the potent, addictive pain killer, and addictive it was.
I’ve been a recovering alcoholic since 1982. I understand addiction and I understood quite well that I had become dependent on the narcotic. I no longer really needed it for the pain for which it was prescribed, I needed it for the pain caused by the withdrawal you experience between “hits.” When you are taking pain killers there’s a simple question you must ask yourself every time you reach for a pill. “Am I taking this because I need it for pain or am I taking it because I want it?” If you are truthful with yourself and the answer is the latter, you have a problem. I had a problem. By addict standards I wasn’t taking much Oxycontin, only about 30-40 milligrams a day, but it was enough for me to know I needed the drug, needed it not to get high…I needed it to feel normal. That’s what happens to every drunk and junkie…they ultimately drink, shoot or take pills just to try to feel normal. Often the first high you have, is the last one.
Having been through chemical dependency treatment in 1982 I knew what I had to do but I also knew I couldn’t do it cold turkey. I found a highly reputable pain clinic that specialized in addiction and started going there. They immediately took me off of Oxycontin and put me on Suboxone another addictive drug but one that is used to slowly help people through the painful withdrawal that comes with quitting. It took several months but it worked and I was Oxycontin free but, sorry, the story doesn’t end there.
You’d think that after having survived cardiomyopathy, getting a heart transplant, beating terrible pain and withdrawing from an addictive drug I would finally feel better. Unfortunately the light at the end of my tunnel was an oncoming train that hit me hard and almost had me down for the count because for no explainable reason I fell into a deep, dark depression that lasted for a couple of years.
Each day I would awaken, head to my favorite recliner in a corner of the den and sit there in the dark drinking coffee and watching TV. I was nearly a zombie. Some days I wouldn’t even shower and I didn’t want to see or talk to anyone. That was my life day after day, week after week for a couple of years. Depression is one of those diseases where you don’t know how bad off you are until you are no longer bad off. The only thing that gave me any hope each day was maintaining my presence on the Facebook group I started, Organ Transplant Initiative and my blog on WordPress, Bob’s Newheart. While I knew I needed professional help I was so depressed I didn’t’ care if I got it so I kept putting it off. Finally with Robin’s gentle prodding I went back to Mayo and began treatment but you don’t beat depression overnight or even in a few months. Sometimes it takes a considerable amount of trial and error before the right treatment is found. That came right around my four year post surgery mark but not until i had lost 75 pounds from lack of appetite. i was left weak but finally energized and optimistic again.
Through all of that Robin, the lunatic who married a dying man, was steady as a rock. She had her hands full running two businesses and our home plus being my caregiver. I’ll never know how she did it and kept her wits about her but she never flinched. She is the most amazing, compassionate and competent human being I have ever encountered. She is an unflappable optimist who doesn’t have a selfish bone in her body. I don’t know why I was so blessed to find this woman but as the man said, “Somebody up there likes me.”
That takes us to today…five plus years later and I feel wonderful but most importantly I get to spend time with Robin. If a physician could have written a prescription for love, happiness and contentment it would simply have said, “Robin.” It is only because of my donor that I am getting to spend time with this wonderful, gracious, smart, talented, funny and super woman. The heart of a stranger has allowed us to really get to know each other. There is no greater gift my donor could have given me and yes, that’s selfish but in this case I think selfish is OK.
Like many recipients my life has changed in other ways as well. Because of a transplant I’m a different person. I hope I’m a better person. I know I appreciate life a great deal more than I ever did before, but it is not only my life I appreciate, it is everyone’s life. When you experience death or near death, “life” takes on a whole new meaning. My reaction to being a transplant recipient is that I owe my donor big time. While I can’t do anything for him directly I can honor his memory by doing everything in my power to help others live. That’s why I am such an outspoken donation/transplantation activist.
While science generally rejects the notion, some recipients feel they have taken on some of the characteristics of their donor. I can’t say what my donor’s characteristics were because I didn’t know him but my life has changed as a result of having his heart. He may well be the influence behind some of the changes I have experienced which include:
- I am much less selfish than I was before and spend as much time as I can trying to help others.
- I am much less concerned with material things than I used to be. “Appearances” aren’t important anymore. I don’t have to have a new car, wear the best clothes or get recognition. I simply don’t care about those things.
- I am far more passionate about causes I believe in like fairness, equality and justice. I particularly feel a need to help the economically disadvantaged, the disabled, the sick, the elderly and, of course — children who suffer so many indignities of which they should not even be aware, never mind being forced to experience them.
- I am more of a peacemaker. In the past I was a warrior, a bulldozer who when advocating for a cause would show my commitment by rolling over those who disagreed and sometimes belittling them in the process. Now I believe in finding common ground and forming friendships despite serious disagreements.
- I am much less self-centered than I used to be. I have come to accept who I am and as a result can concentrate on the needs of others.
- I have always enjoyed learning but it has almost become an obsession since my transplant. My thirst for knowledge about a wide variety of things knows no bounds. I can’t get enough information about the wonders around us like the sun and the stars and the miracles, medical and otherwise that we experience every day.
- Working with my hands has always been enjoyable for me but since my transplant I have become addicted to woodwork. I’m not the Michelangelo of woodworking, hell I’m not even a Barney Fife but I am determined to get better at it. Unfortunately it is my friends and family who must suffer receiving my woodworking “gifts” and then acting as though they like them.
Being a transplant recipient is an amazing experience. It is one of which I am always aware and I mean always that I have someone else’ heart. There is no time in my waking hours that I am not aware that I am alive because a generous stranger give me his heart. I owe him and his family more than I could ever repay no matter what efforts I make for the rest of my life.
If you, the reader, are an organ donor, let me thank you on behalf of the unknown lives you may save as a result of your selfless action. If you are not an organ donor, please consider it carefully. You can save or enhance the lives of up to 60 people just by signing up and you can do that so easily. Just go to www.donatelife.net and follow the directions. Then, tell your family what you’ve done so there is no chance that anyone will object when the time comes to fulfill your commitment.
Earlier in this story I mentioned my Facebook Group and Blog. Let me take just a moment to explain how they came to be. Just a couple of months after my transplant I got a call from Mayo asking if I’d be interested in starting a Facebook Organ donation group and in writing a blog. I knew what neither were but decided I needed something to do during my recuperation and said, “Yes.” With Mayo’s help I got started immediately.
That was the beginning or Facebook’s Organ Transplant Initiative group (OTI) and Bob’s Newheart blog on WordPress www.bobsnewheart.wordpress.com . OTI now has almost 2,500 members and I’ve posted 140 blogs on donation/transplantation issues that have been read by over 100,000 people in at least 20 countries. I believe that I was given my new heart to do this and it has become my new passion.
None of this would be possible without all you wonderful people who helped to make OTI a success and who read my “Stuff” on WordPress. By offering your kind words, thoughts and deeds you are doing a great service to those who suffer while waiting for organs and those who are recovering from receiving them, never mind the caregivers and others who are so critical to the donation/transplantation process. Words cannot express my fondness for all of you and my gratitude for your involvement. All I can say is, thank you from the bottom of my donor’s heart.
Bob Aronson of Bob’s Newheart is a 2007 heart transplant recipient, the founder of Facebook’s nearly 2,500 member Organ Transplant Initiative and the author of most of these donation/transplantation blogs.
You may comment in the space provided or email your thoughts to me at bob@baronson.org. And – please spread the word about the immediate need for more organ donors. There is nothing you can do that is of greater importance. If you convince one person to be an organ and tissue donor you may save or positively affect over 60 lives. Some of those lives may be people you know and love.
Please view our video “Thank You From the Bottom of my Donor’s heart” on http://www.organti.org This video was produced to promote organ donation so it is free and no permission is needed for its use.
If you want to spread the word personally about organ donation, we have another PowerPoint slide show for your use free and without permission. Just go to http://www.organti.org and click on “Life Pass It On” on the left side of the screen and then just follow the directions. This is NOT a stand-alone show; it needs a presenter but is professionally produced and factually sound. If you decide to use the show I will send you a free copy of my e-book, “How to Get a Standing “O” that will help you with presentation skills. Just write to bob@baronson.org and usually you will get a copy the same day.
Also…there is more information on this blog site about other donation/transplantation issues. Additionally we would love to have you join our Facebook group, Organ Transplant Initiative The more members we get the greater our clout with decision makers.
Yes, Brain Death Means You Are Really Dead!
Are brain dead patients really dead? That’s the question many people are asking because of stories circulated by irresponsible journalists, TV shows and movies who seek sensational plots and people who just refuse to acknowledge the facts.
The simple answer to this question is, “Absolutely. If you’ve been declared brain dead by a qualified team of experts in a hospital setting then you are dead. The New York Organ Donor Network put it best, “There are more tests to establish death done on potential organ donors than there are on people who are not donors.”
There have been several stories circulated about how “Brain Dead” people have recovered and gone on to live normal lives. I have spent the last month looking into these stories and have determined that while one or two are unexplainable primarily because families won’t release medical information all the rest were simply not true.
I have interviewed two world famous neurologists who have written extensively about brain death and who were part of the process that developed the rules for making that determination. The protocols for determining brain death are more rigorous than for proclaiming death under normal circumstances. Every single neurologist, physician or other medical expert I’ve talked with has said the same thing, “No one recovers from brain death!” New protocols were established in 2010 to make the testing even more rigorous and they require the physician who is declaring brain death to fill out a check list to be sure every step has been completed. Again, this process is more rigorous than what is used to declare death under normal conditions.
Here’s the checklist that must be followed in order to declare brain death:
Cause of Brain Death:
________________________________________________________________
Date of Exam: ____________________________
Time of Exam: ____________________________
A. Absence of Confounding Factors: RESULTS
1. Systolic blood pressure > 90 mmHg ______________________
2. Core temperature > 36˚C ______________________
3. Negative for drug intoxication or poisoning _______________________
4. Toxicology results ______________________
5. Negative for neuromuscular blocking agents ______________________
B. Cranial Nerve Reflexes and Responses:
1. No spontaneous muscular movements ______________________
2. Pupils lightfixed
_______________________
3. Absent corneal reflexes ______________________
4. Unresponsiveness to intensely painful ______________________
stimuli, e.g. supraorbital pressure
5. Absent response to upper and lower ______________________
airway stimulations, e.g. pharyngeal and
endotracheal suctioning
6. Absent ocular response to head turning ______________________
(no eye movement)
7. Absent ocular response to irrigation of the ears ______________________
with 100 mls. of ice water (no eye movement)
8. Apnea PaCo2>60 mmHg ______________________
a. PaCo2 at end of apnea test
b. PaO2 at end of apnea test
C. Medical Record Documentation of the above Examination
D. Comments
__________________________________________________________________________
__________________________________________________________________________
__________________________________________________________________________
__________________________________________________________________________
________________________________
Certification of Death
Having considered the above findings, we hereby certify the death of:
_____________________________________________________________________________
Physician Signature Printed Name Date/Time
There will always be naysayers and people who “know of people who recovered” but I am satisfied after considerable research that when brain death is declared it is final.
Brain death is never declared by anyone with any connection to organ recovery and transplantation. The transplant team is not even aware of the patient until after brain death has been declared. The physician who declares brain death is independent of the recovery and transplantation team. Physicians who attend to patients on a regular basis are sworn to and legally committed to do everything possible to save your life. They are not part of the transplant team either and in many cases the hospitals where people are declared brain dead don’t even have transplant teams because they are not transplant centers.
To add to theevidence I have offered is this information from Stacey Gelowitz Renal Transplant Coordinator at Alberta Health Services Edmonton, Canada Area Hospital & Health Care. While she is in Canada the American and Canadian processes for declaring brain death are virtually identical. Here’s what she wrote:
“At our center, we define neurological death by two criteria: irreversible loss of the capability for consciousness AND irreversible loss of all brainstem functions (including breathing). The protocol we follow for adult NDD is as follows:
Done twice by 2 physicians independently, who are not associated with transplantation
(1) Deep unresponsive coma with known cause
(2) Absence of confounding factors (eg. alcohol, tricyclic antidepressants)
(3) Temp > 34 degrees C
(4) No brainstem reflexes
a. No motor responses except spinal reflexes
b. No cough
c. No gag
d. No corneal responses bilaterally
e. No vestibulo-ocular responses bilaterally
f. No oculocephalic reflex (Doll’s eyes test; contraindicated in spinal injury)
g. No pupillary response to light bilaterally (pupils 6mm)
h. Apnea test, pH < 7.28 and PaCO2 > 20mmHg above pre-apnea test level
(5) If pt doesn’t meet all above criteria, do ancillary tests to show absence of intracranial blood flow:
a. Radionuclide cerebral blood flow study
b. Cerebral angiography
It can be hard for families to comprehend that their loved one is dead because the heart continues to beat spontaneously and the person is supported by machines so they look asleep. Important to note is that…
* No brain function remains (in contrast to coma/vegetative state).
* Heart continues to beat because of mechanical support stabilizing body, e.g. ventilators. Remember: Sinus rhythm is controlled by cells within the heart (SA/AV nodes), so as long as the heart is being perfused adequately (getting O2 via blood), it is happy to continue beating. Medulla oblongata in brain controls rate and strength of beat, but not basic rhythm).
* Blood still flowing to body organs (heart, lungs, liver, kidneys, pancreas) allowing transplantation if donor family consents, the organs are functioning adequately, and the potential donor has no serious health concerns
It is VERY IMPORTANT that the donor does not have any factors that confound the diagnosis of brain death. I think it is in these circumstances that brain death is (very rarely) wrongly diagnosed. A great website that you can refer to that touches on these ideas: http://www.braindeath.org/clinical.htm. It goes through different confounding factors and why physiologically in their presence brain death cannot be declared.
I have not seen any reports where pts recover from ‘brain death’ and it was not due to one of these confounding factors. We have gotten much better as a medical community at recognizing the suppressive effects of this list and know now not to declare brain death in the their presence. I think where patients extremely rarely slip through that can lead to wrong diagnosis of brain death is in the following two circumstances: (1) pts are on an unknown substance that is not tested for on toxicology panels and suppresses brain stem reflexes. Or, (2) a pt receives a drug in hospital (eg sedative to stop seizures or allow intubation) and the pt metabolizes the drug extremely slowly. The latter example (slow drug metabolism) is more applicable to children/babies rather than adults, but can happen in both (here is a case study from our center describing just that: http://www.ncbi.nlm.nih.gov/pubmed/19818943). As a result, the time in which brain death is declared was extended.
People need to understand that these instances are incredibly rare. If there is any doubt that one of these confounding factors is contributing to a wrong diagnosis of brain death, another tox screen or temp etc can be done to rule out such factors. Take a look at the cases people are presenting on reversible brain death. I would bet that all fall under what is discussed above. That said, some people will still stick to their guns and not believe you no matter how much info is provided, and that’s okay too”
If anyone needs more information that I have provided here I suggest you contact a neurologist at your nearest transplant center and ask him or her. If you still doubt the process then perhaps you should not be a donor.
Bob Aronson is a 2007 heart transplant recipient, the founder of Facebook’s 1700 member Organ Transplant Initiative and the writer of most of these donation/transplantation blogs on Bob’s Newheart.
You may comment in the space provided or email your thoughts to me at bob@baronson.org. And – please spread the word about the immediate need for more organ donors. There is nothing you can do that is of greater importance. If you convince one person to be an organ and tissue donor you may save or positively affect over 60 lives. Some of those lives may be people you know and love.
Please view our video “Thank You From the Bottom of my Donor’s heart” on http://www.organti.org This video was produced to promote organ donation so it is free and no permission is needed for its use.
If you want to spread the word personally about organ donation, we have a PowerPoint slide show for your use free and for use without permission. Just go to http://www.organti.org and click on “Life Pass It On” on the left side of the screen and then just follow the directions. This is NOT a stand-alone show, it needs a presenter but is professionally produced and factually sound.
Also…there is more information on this blog site about other donation/transplantation issues. Additionally we would love to have you join our Facebook group, Organ Transplant Initiative The more members we get the greater our clout with decision makers.


You must be logged in to post a comment.